Meniscus tear: Surgery, rehabilitation, costs
- Cause and progression of a meniscus tear
- When does a meniscus injury require surgery?
- What happens before surgery for a meniscus tear?
- How is meniscus surgery performed at Gelenk-Klinik?
- Which type of physician operates on a torn meniscus?
- What type of anaesthesia is used for meniscus surgery?
- After-care, rehabilitation and aids following meniscus surgery
- Should I expect pain after meniscus surgery?
- What will my stay be like at Gelenk-Klinik?
- What do I need to keep in mind after meniscus surgery?
- Cost of an arthroscopic knee surgery
- How can international patients schedule meniscus surgery?
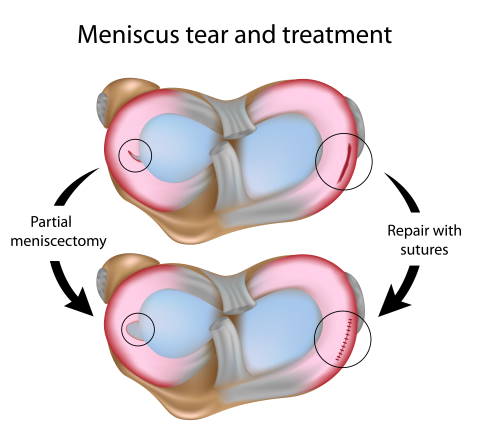 A torn meniscus can be operated on in two different ways. In meniscectomy, the surgeon removes part of the damaged meniscus to smooth the surface. In meniscal suturing, the damaged part of the meniscus is sutured back in order to achieve healing of the fragments. Suturing the meniscus is only possible if the torn meniscus is close to the base of the meniscus, which is well supplied with blood. © Alila Medical Media
A torn meniscus can be operated on in two different ways. In meniscectomy, the surgeon removes part of the damaged meniscus to smooth the surface. In meniscal suturing, the damaged part of the meniscus is sutured back in order to achieve healing of the fragments. Suturing the meniscus is only possible if the torn meniscus is close to the base of the meniscus, which is well supplied with blood. © Alila Medical Media
A meniscus tear is one of the most common knee joint injuries. Any accident that leads to a forceful twisting or bending of the knee joint can cause a meniscus tear. The risk of injury is greater the more weight or speed is applied to the knee at the moment of injury. The more the knee joint is rotated inwards and bent into a knock-knee position, the greater the risk of a meniscus injury.
The knee joint has a medial and a lateral meniscus. These are half-round fibrocartilaginous soft tissue structures located between the shinbone (tibia) and thigh bone (femur) and work like shock absorbers. An acute meniscus tear will immediately cause sharp pain, swelling of the knee joint, and noticeable restriction in motion when bending or extending it. Sometimes the knee seems “locked”. On the other hand, a meniscus that has worn over time will gradually cause symptoms such as stress-related pain and the knee will occasionally lock up.
In some cases, a meniscus tear will heal on its own with immobilisation, rest and physiotherapy. When there is chronic pain or the knee locks up, meniscus surgery can help resolve the problem.
Cause and progression of a meniscus tear
A meniscus tear can always occur if the knee is forcefully twisted or bent. Even simply overloading the knee joint during very fast start-stop movements or violent rotations can overstrain the meniscus and lead to a meniscus tear.
Meniscus tear during sports
A meniscus tear often occurs e.g. whilst skiing, if the ski catches. At full speed, the kinetic energy of the body causes the knee joint to twist. Even during football, basketball and other so-called contact sports, the high rate of acceleration and often great, uncontrollable external forces (opponents) can cause this type of injury.
Meniscus tear at work
Many professions are very hard on your menisci. Occupational activity that includes working in a squatting position (e.g. when tiling) can cause strain. The extreme flexion of the knee joint and the force of body weight exert strong forces on the meniscus and knee pain is the result.
Another cause for problems is the heavy lifting of loads from a squatted position. What is essentially a back-friendly recommendation for such work puts a strain on the meniscus. If the knee is already damaged, you have the choice of overloading either the meniscus or the intervertebral discs.
Degenerative meniscus tear in elderly patients
The meniscus in older patients often exhibits degenerative damage. Since the tissue is fibrocartilaginous (similar to cartilage), it is subject to high levels of wear. If this wear is already advanced, even minimal strain is often enough to cause a meniscus tear.
We have to take such pre-existing conditions into account when deciding on the treatment. Fully reconstructing a meniscus with pre-existing degenerative damage is not a simple task.
In younger patients it usually takes a traumatic injury involving great amounts of force to cause a meniscus tear. If the meniscus is already damaged in elderly patients, a simple awkward movement or a stumble can be enough to cause it.
Orthopaedic risk factors of a meniscus tear
Any regular strain on the knee joint can also weaken the menisci. Being overweight is therefore one of the main risk factors for a meniscus tear or meniscus degeneration (wear). A malalignment of the knee joint - due to, for example, being knock-kneed or bow-leggedness - can change the forces applied to the knee joint to cause parts of the menisci to degenerate faster.
A prior cruciate ligament rupture strains the menisci. the cruciate ligaments center the femur and tibia in the knee. If a cruciate ligament is torn, all shear forces, acceleration forces and braking movements act directly on the menisci without being slowed down by the cruciate ligaments, which act like safety belts.
Since meniscus tears often cause impingements, edges, irritation and movement disorders in the knee joint, those affected should seek an orthopaedist as soon as possible. A visible sign of meniscus damage is a painful, swollen Baker's cyst at the back of the knee due to inflammatory irritation of the joint capsule. Meniscus surgery is oftentimes only suited to prevent subsequent damage such as joint wear and arthrosis. An experienced diagnostician and knee specialist can assess whether a meniscus tear can heal on its own or requires surgery.
When does a meniscus injury require surgery?
A meniscus tear doesn’t always require surgery. Depending on the type, size and location of the tear, the patient’s age, or the condition of the meniscus tissue, in some cases there is a good chance it will heal on its own.
A torn meniscus needs surgery if the nature of the injury leaves no prospect of the meniscus healing with physiotherapy alone. The goal of meniscus surgery is to ensure that the knee joint remains pain-free, resilient and functional in the long term. It is designed to recover resilience in everyday life and during sports. A strong, intact meniscus also prevents degenerative changes from straining the cartilage surface in the knee joint (arthrosis).
Surgery in younger patients with meniscus tear
It is typically relatively easy to determine whether younger patients with traumatic meniscus tears require surgery:
- Persistent pain following a meniscus tear
- Knee locking up
- Flap tear in the meniscus
- Meniscus damage in the inside (intermediate) area
Surgery for degenerative meniscus tears in elderly patients
It is a bit more complicated when it comes to degenerative changes. Depending on how extreme the restriction of motion and symptoms are, an attempt can be made to delay surgery with conservative treatment options. Even in the case of meniscus tears caused by degeneration - i.e. wear and tear - it can be important to smooth the joint surface and free the knee joint from cartilage-damaging blockages before knee arthrosis occurs.
What happens before surgery for a meniscus tear?
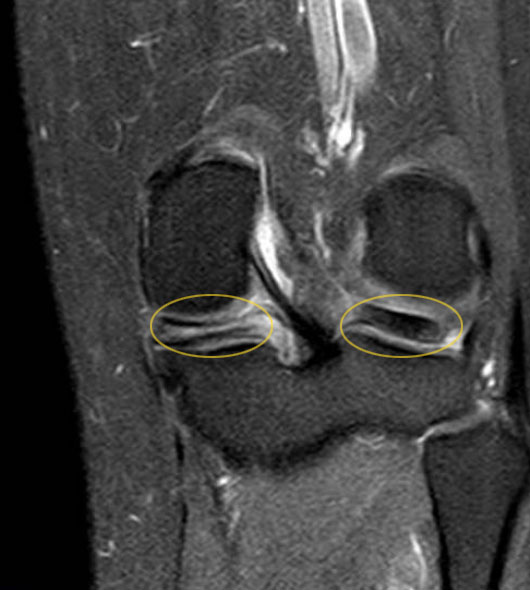 The knee injury shows a clear horizontal meniscus tear along the longitudinal axis (yellow marking on the left). The other meniscus in the knee joint (marked on the right) is still intact, clearly visible by the larger dark area. © joint-surgeon
The knee injury shows a clear horizontal meniscus tear along the longitudinal axis (yellow marking on the left). The other meniscus in the knee joint (marked on the right) is still intact, clearly visible by the larger dark area. © joint-surgeon
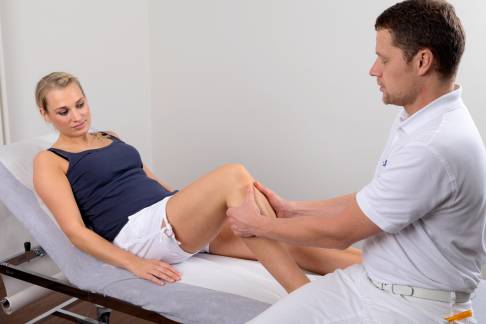
Prior to surgery, the physician will conduct detailed medical diagnostics. The knee specialist can essentially already establish a meniscus tear based on questions for the patient (medical history) and a physical examination. During the medical examination the specialist will test the knee joint’s range of motion in different positions. They will assess the gait as well as flexion and extension. A torn meniscus causes relatively noticeable pain, particularly in the joint space of the knee joint, which already provides fairly good clinical support for the diagnosis.
X-rays are always taken in the case of knee pain because they help the knee specialist examin the patient to assess the overall situation in the knee joint. The standing x-ray provides an indication of the thickness of the cartilage layer. In this way the physician can, for example, rule out knee arthrosis as the cause of the sharp pain. Even bone injuries are possible, accompanied by damage to the knee joint caused by distortion (twisting) or buckling. The x-ray can be used to rule out bone injuries or fractures.
Unlike the x-ray, which primarily shows bones, an MRI (magnetic resonance imaging) shows detailed images of all soft tissue. This allows the knee specialist to assess the condition of tendons, ligaments and fibrocartilaginous menisci. Particularly valuable in the MRI examination of a torn meniscus is the possibility of displaying the course, length and exact location of the meniscus damage in detailed imaging.
How is meniscus surgery performed at Gelenk-Klinik?
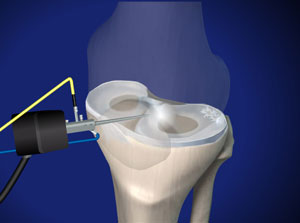 Knee specialist approach to arthroscopic meniscus repair ©Viewmedica
Knee specialist approach to arthroscopic meniscus repair ©Viewmedica
If the patient is suffering from severe pain or restriction of motion, immediate meniscus surgery is often required. All meniscus surgeries are arthroscopic, so minimally invasive. The surgeon only makes small incisions on both sides of the knee joint, next to the patella, to insert the arthroscope and the surgical instruments through small tubes. The minimally invasive access speeds up healing and reduces the risk of complications.
There are generally two types of meniscus surgery: meniscus repair and meniscus removal (meniscectomy).
Meniscus repair
If the tear is new – particularly near the capsule, hence well perfused area (meniscus base) – the otherwise healthy meniscus tissue is best repaired with sutures. Especially in the lateral and frontal areas, perfect arthroscopic sutures are achieved with modern techniques and the use of special sutures. Here the surgeon determines the suture technique based on the size and location of the tear for optimal meniscus repair.
Even in the relatively severe so-called bucket handle tears with large-area tears, the meniscus should be preserved as far as possible by suturing in order to reduce the risk of arthrosis.
Rehabilitation period following meniscus suturing
After meniscal suturing, the patient is restricted in the movement of the knee joint for about six weeks, but may put full weight on it. This means that full weight bearing is permitted immediately after the operation, but only at full extension. As soon as the knee joint is bent, it must not bear weight, as the meniscal suture could tear open due to the high shear forces.
A special brace (orthosis) that can be locked at full extension ensures this type of weight bearing. To bend the knee (e.g. whilst sitting), it can be unlocked and the knee joint can be bent without weight bearing. The patient should refrain from sports for six to eight weeks after a meniscus repair. Sports that put a strain on the knee joint should not be pursued before six months have elapsed and following consultation with the surgeon.
Partial meniscus removal (partial meniscectomy)
If the shape and location of the meniscus tear indicate that conservative treatment or suturing is unlikely to be effective, the torn section must be removed. The resection smooths the joint surface and extends the life of the joint cartilage. Even with a partial meniscectomy, it is very important to preserve as much of the meniscal tissue as possible. The larger the preserved portion of the meniscus, the more meniscus function is retained.
Rehabilitation period following meniscectomy
After a partial meniscectomy, the patient will already be permitted partial weight bearing the day of surgery. Forearm crutches help control this weight bearing. A meniscectomy typically requires one to two weeks of sick leave. If the patient's professional activity places particular strain on the knee, a longer period of sick leave may be necessary.
After one week, the patient can already carefully commence with "gentle" sports, i.e. sports that do not put too much strain on the knees, such as cycling. Swimming is typically only permitted once the wound is fully healed and the sutures have been removed.
Three to four weeks after a meniscectomy, the patient can even return to more strenuous sports such as football, tennis or jogging.
Meniscus replacement and synthetic meniscus for meniscus tear
The meniscus of an organ donor can be transplanted for a meniscus replacement. In younger patients with major meniscus damage, a meniscus replacement is often the only option to prevent early joint wear in the knee. Even an artificial meniscus made from synthetic materials can be implanted.
Both the transplantation and the insertion of synthetic material are so-called ''exceptional interventions''. They usually result from previous, possibly failed operations on the meniscus, which were not able to maintain meniscal function.
Often, too much meniscus tissue was removed, or too soon. Although the results of the transplantation of synthetic implants of the meniscus are promising, so far there are not enough reliable long-term results for this procedure.
These interventions should therefore not be considered from the outset as a first choice of treatment. It’s therefore important for patients to seek a qualified knee specialist as soon as possible following a meniscus injury. The specialist will be able to quickly make a reliable diagnosis and determine the necessary treatment options. The goal must always be to preserve as much of the natural meniscus tissue as possible, thus meniscus function, to avoid a meniscus replacement.
Meniscus replacement: meniscus tear surgery implanting a donor meniscus
If the meniscus cannot be repaired, either due to the location and size of the tear, or because a lot of the meniscus was previously removed, a donor meniscus can be implanted. This solution is often used to prevent early arthrosis and early cartilage damage in young patients.
Both the medial and the lateral meniscus can be replaced. However, it’s important to first determine the exact size and location of the meniscus being replaced. The necessary donor meniscus comes from an international transplant centre. There is often a long wait before a match is found. Due to various administrative obstacles, there currently is no German donor system for meniscus tissue with a German tissue bank. The meniscus tissue is primarily imported from Benelux countries. Fortunately, these transplants do not cause the rejection reactions organ transplants are known for.
Since the implant is harvested under sterile conditions and examined for germs there are virtually no infections from the donor meniscus.
The minimally invasive procedure during which the surgeon implants and affixes the prepared meniscus implant through a tiny access typically takes about two hours.
Synthetic meniscus implant
Synthetic meniscus tissue is mainly used to repair partial injuries and damage to the medial and lateral meniscus. This new, spongy material has a porous structure, making it particularly suitable. Vessels can grow into the dense pore structure to stimulate growing endogenous tissue. Once the new natural tissue starts taking on its function, the implant dissolves and is broken down by the body. This procedure is also minimally invasive, i.e. using a small incision to ensure maximum preservation of the healthy tissue.
Which type of physician operates on a torn meniscus?
Here at Gelenk-Klinik we believe a close relationship between the physician and their patient is important. This means you will be in the care of your treating physician from the initial appointment until after the meniscus surgery. This physician is also responsible for your aftercare. So, you will have one contact person who will be assigned to you throughout your stay at Gelenk-Klinik. Our knee specialists are Professor Sven Ostermeier and PD Dr Bastian Marquaß.
What type of anaesthesia is used for meniscus surgery?
Meniscus surgery is typically performed under general anaesthesia. However, we also offer spinal anaesthesia to avoid the risks of general anaesthesia. In the case of spinal anaesthesia, an anaesthetist injects the anaesthetic into the spinal canal of the lumbar spine. The patient is fully conscious during surgery. Our anaesthetists are very experienced in both methods and choose the option best for you and your circumstances during a mutual pre-operation discussion.
After-care, rehabilitation and aids following meniscus surgery
The first week following meniscus repair surgery, the knee will be immobilised with a special brace. You will further receive forearm crutches to use for about 6 weeks to reduce strain on the knee. After this, weight bearing will gradually be increased until full weight bearing is reached. During the partial weight bearing period, thrombosis prophylaxis (e.g. Heparin/Enoxaparin) is vital. You should also wear compression socks until full weight bearing has been restored. We will ensure you receive the aid required after surgery.
Should I expect pain after meniscus surgery?
Every surgical procedure may cause pain. We always try to minimise this pain as much as possible. The anaesthetist often uses a so-called nerve block before the surgery, numbing the respective knee for about 30 hours. This already manages the immediate wave of pain after surgery, which can then be easily treated with regular medication. Our goal is for you to experience as little pain as possible.
What will my stay be like at Gelenk-Klinik?
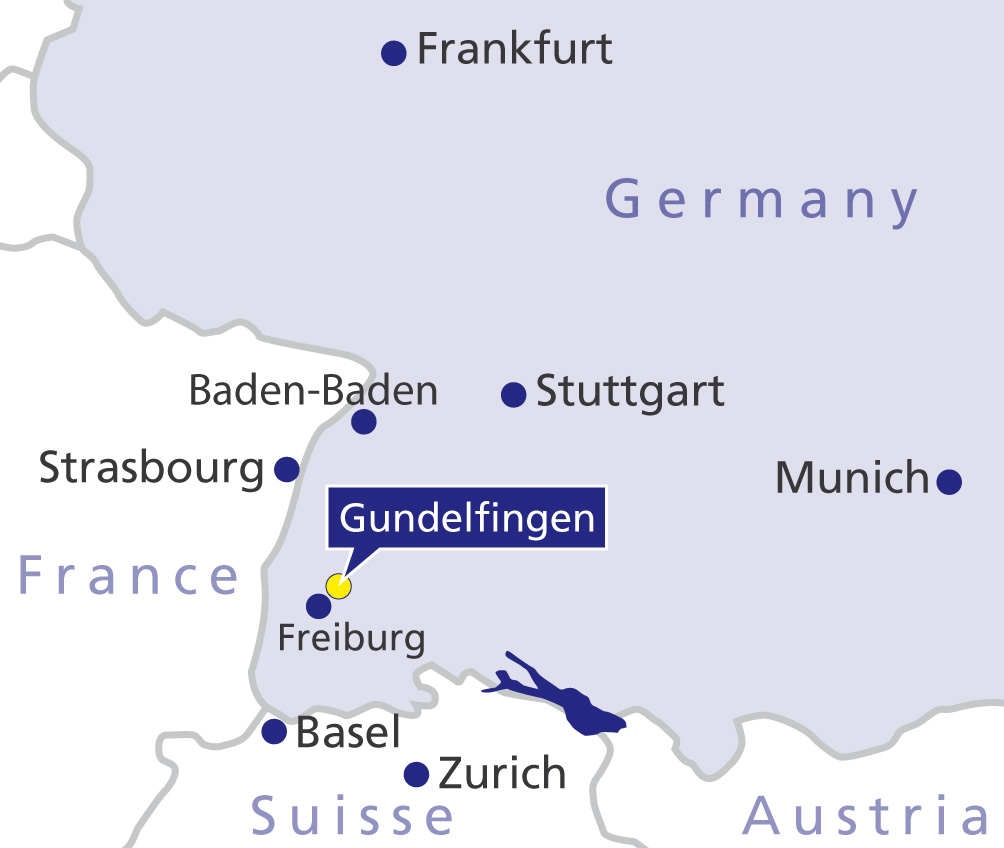
 Private room in the Gelenk-Klinik in Gundelfingen, Germany
Private room in the Gelenk-Klinik in Gundelfingen, Germany
During your inpatient stay at Gelenk-Klinik you will have a single-occupancy room. The room has a bathroom with a shower and WC. All rooms include towels, a bath robe and slippers. They further include a mini-bar and safe. All rooms also have a television. You only need to bring your personal medication, comfortable clothes and sleepwear. After surgery you will receive 24-hour care from experienced nursing staff, an international patient care team and experienced physiotherapists. The inpatient stay following the procedure typically lasts 3 days. Your family members can stay at a hotel within walking distance (300 m). We will help you to make the reservations.
What do I need to keep in mind after meniscus surgery?
You should elevate and ice your knee immediately after the procedure. The sutures will be removed about 5 days after surgery. At that point you may shower again.
To avoid complications, you should rest your knee for a few weeks after meniscus surgery. Your sick leave may be up to 6 weeks depending on your occupation. You will receive a written sick note from us for this time. It’s vital to use thrombosis prophylaxis until your leg returns to full weight-bearing. Extensive physical therapy is vital during this time to prevent muscle loss and the function of the knee.
You should schedule your return flight no earlier than 7 days after surgery. We recommend optimally waiting about 10 days.
- Inpatient treatment: 3–4 days
- Optimal local stay: 10–14 days
- Earliest return flight: 7 days after surgery
- Recommended return flight: 10 days after surgery
- Showering permitted: 5 days after surgery
- Recommended time off work: 2–6 weeks (depending on occupation)
- Recommended removal of sutures: 5 days
- Outpatient physiotherapy: 2 weeks
- Time before being able to drive again: 6 weeks
- Low-impact sports: at least 8 weeks after surgery
- Regular sports: 6 months after surgery
Cost of arthroscopic knee surgery in Germany
In addition to the cost of surgery, you will also need to plan for additional costs for diagnostics, physician’s appointments and aids (e.g. crutches). These will be about 1,500 to 2,000 Euro. If you plan to have outpatient physiotherapy after surgery, we will gladly send you an estimate of costs.
You will find information about the cost of hotel lodging and any follow-up treatment at the rehabilitation clinic on the websites of the respective providers.
How can international patients schedule meniscus surgery?
We will first need recent MRI images and x-rays to medically assess the condition of your knee. After sending these to us via our website, we will send you patient information and a binding estimate of costs within 1–2 days.
Gelenk-Klinik offers quick appointments to accommodate your preferred travel itinerary. We will gladly help you apply for a visa once we have received the down-payment specified in the cost estimate. If the visa is denied, we will refund the full down-payment.
We try to minimise the time between the preliminary examination and the surgery for our international patients to avoid additional travel. During your inpatient and outpatient stay our multi-lingual (English, Russian, Spanish, Portuguese) case management team will be there to assist you. We can also provide an interpreter (e.g. Arabic) at any time, at the patient’s expense. We will gladly assist you with organising transportation and lodging and provide tips for recreational activities for your family members.