Disc Protrusion or Disc Herniation: Percutaneous Endoscopic Disc Nucleoplasty (Thermo Ray)
Key Facts of Endoscopic Nucleoplasty
- Indication: Painful spinal disc protrusion
- Strategy: A small tube is inserted into the affected disc. This tube reduces tissue volume, by generating a high-frequency, electro-thermal field, in the liquid core of the intervertebral disc.
- Inpatient treatment: 2 days
- Rehabilitation treatment: 14 days outpatient rehabilitation
- Earliest flight home: 3 days after surgery
- Recommended flight home: 14 days after surgery
- Time before showering: 1 day after surgery
- Recommended time off work: 2 weeks
- Time before driving a car: 1 week
What is Percutaneous Disc Nucleoplasty?
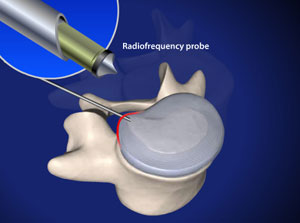 Percutaneous Disc Nucleoplasty: Intradiscal Electrothermal Therapy is designed to reduce the tissue volume of the spinal disc by evaporating part of the liquid core, this lowers the pressure on the walls of the spinal disc, which in turn reduces the painful protrusion of the disc. The pain related to bulging spinal disc walls will subside after the surgery. © Viewmedica
Percutaneous Disc Nucleoplasty: Intradiscal Electrothermal Therapy is designed to reduce the tissue volume of the spinal disc by evaporating part of the liquid core, this lowers the pressure on the walls of the spinal disc, which in turn reduces the painful protrusion of the disc. The pain related to bulging spinal disc walls will subside after the surgery. © Viewmedica
Percutaneous Disc Nucleoplasty is a minimally invasive surgery to reduce the volume of a bulging or herniated disc. In both cases, the spinal disc puts pressure on a nerve root or the spinal cord and causes back pain or sciatic pain.
Spinal Disc Protrusions do not require open spine surgery
Many patients with back pain show no clear indication of a herniated disc. However, with MRI investigation protrusion of the intervertebral discs can be diagnosed. This protrusion can put pressure on nerves or the spinal cord and can cause persistent, or stress-related chronic back pain. Normally this kind of back pain (lumbar or cervical), responds well to conservative treatment options.
When will your neurosurgeon consider Nucleoplasty?
Conservative Treatment of Disc Protrusions
- Physiotherapy and strengthening exercises
- Physical Therapy
- Weight reduction
- Treatment with painkillers
For a thorough investigation and to discuss conservative treatment options, please contact our back and spine department.
If after six weeks, conservative treatment has not been successful, your spine specialist should consider an intradiscal procedure: The disc protrusion can be reduced by treating the liquid core of the spine simply by using an injection needle. This needle (cannula) allows a radiofrequency instrument to enter the core of the disc, thereby avoiding all the surgical risks associated with open back surgery. This is essentially the principle of Nucleoplasty.
Nucleoplasty, as a minimally invasive treatment, covers only smaller disc herniations or disc bulges that have not yet broken through the solid fibre ring of the disc and are therefore not accessible via an open surgical procedure (surgical removal of the disc material).
Internationally, more than 200,000 patients have already been treated with nucleoplasty, with a greater than 80% success rate.
Endoscopic Nucleoplasty is safe for patients and is a minimally invasive procedure, which produces very good outcomes, without the risks and postsurgical complications associated with open back surgery.
What is the principle of Nucleoplasty by thermal coblation?
Terminology
- Nucleoplasty: Changing the shape or volume of the liquid core (nucleus) of a spinal disc
- Coblation: Short for controlled ablation (removal or reduction of disc material). Coblation® is a patented and registered procedure.
- Disc herniation: Breach of the fibrous ring around the liquid core of a spinal disc
- Disc protrusion: Bulging of a wall of the spinal disc
- Intradiscal Electrothermal Therapy (IDET): Minimally invasive treatment of disco genic back pain by treating the liquid core of the spinal disc
Nucleoplasty is a minimally invasive method for reducing the internal pressure of the spinal disc.
The high pressure of the liquid core of the disc can lead to protrusion or herniation, particularly if the walls of the disc have already degenerated.
Nucleoplasty by thermal coblation is indicated if there is a significant protrusion with a bulging fibre ring, however, there should not be any evidence of disc herniation which has broken through the disc wall.
The principle is based on a minimal shrinkage of the gelatinous disc nucleus. With the resulting shrinkage, the bulging disc retracts, the compressed nerve is released and the leg pain and back pain subside .
The procedure is called Intradiscal Electro Thermal Therapy (IDET).
Advantages
- Minimally invasive transcutaneous Endoscopic approach: The area around the spinal disc is not traumatized by open surgery, surgery takes place through a needle: muscles, nerves and bones stay intact, and no surgical scar along the spine.
- Studies show a success rate of up to 70% for patients with chronic back pain. With a proper diagnosis, the results are very reliable.
- Easy rehabilitation after IDET treatment: no sutures or scarring in the area around the spine. Patients can go back to work quickly with no postsurgical complications
- The overall stability or mobility of the spine is not affected by Nucleoplasty. Patients do not suffer adverse effects
- Local sedation, avoiding total anaesthesia. The patient is semiconscious during the surgery. This keeps surgical stress at a low level. The procedure takes 20-30 minutes.
- The increase in temperature is controlled and localised, there are no reports of intra or postoperative complications. This contributes to the positive safety profile of radiofrequency Nucleoplasty
Which patients are suitable for Nucleoplasty?
When to look for alternative treatments:
- Facet joint osteoarthritis
- Sequestered Disc herniation
- Loss of disc diameter greater than 50%
- Patients with a high alcohol intake or heavy smokers
- Unstable vertebrate spine (spondylolisthesis)
- Severe spinal stenosis
- Disrupted disc morphology and high-grade disc injury
- Severe neurological symptoms such as loss of urinary control and sexual dysfunction
In this case please contact us to discuss alternative, preferably minimally invasive, treatment options with our spine specialists.
Proper patient selection increases the probability of a good outcome. Patients require a thorough clinical checkup. The stability of the spine should be assessed with dynamic X-ray images. The discs can be investigated in detail via MRI imaging.
Patients should have not more than one affected spinal disc (one segment) at a time. The pain should be caused by disc degeneration only.
Before considering nucleoplasty, a patient should have undergone six weeks of intense conservative treatment, with no improvement in the pain situation.
Conservative treatment should always be the priority in treating disc-related back pain.
Severe stenosis or facet joint degeneration cannot be treated with Nucleoplasty.
The stability of the vertebral spine will also need to be assessed. Patients with spondylolisthesis (instability of vertebrae) are not suitable for Nucleoplasty.
The disc degeneration must not be too advanced. If the disc is already severely collapsed (loss of diameter > 50%) the IDET treatment is not suitable.
Patients with a sequestered disc herniation will also need an alternative treatment approach.
Nucleoplasty by Electrothermal Therapy step by step
Percutaneous Disc Nucleoplasty
Following partial anaesthesia, Specialist Neurosurgeons at the Gelenk-Klinik insert a thin needle through the back and into the herniated disc (x-ray control is used to guide the needle to the required spot).
A small radiofrequency probe is inserted through the needle and into the disc. This device sends pulses of radio waves to dissolve small portions of the disc nucleus.
The temperature applied is low (40°-70°C). The empty space created by this procedure, allows the disc to reabsorb the herniated part of the disc, which in turn leads to pressure relief.
After the needle is removed, the area is covered with a small bandage, no suturing is required.
In detail: How does Nucleoplasty work?
The fibrous ring of the intervertebral disc is strengthened by heating its liquid core. The heat modifies the collagen fibres of the annulus (spinal disc wall): the disc wall contracts and increases in thickness.
The precise mechanism of IDET is still somehow speculative, however, it is considered to decrease discogenic pain by two different mechanisms.
- The thermal modification of the collagen fibres increases the thickness of the annulus ring, thus repairing cracks and degeneration. This effect, which is called disk restructuring, takes place within a few months of the procedure
- Thermal destruction of disk nociceptors: denervation is also a widely used treatment strategy, with the potential of immediate pain relief.
Results of the Nucleoplasty
The chances of success with this method are very good with over 80 % patient satisfaction rates. The precondition for this success rate, however, is a thorough medical investigation and patient selection. The Neurosurgical consultant needs to rule out all other possible causes of back pain.
The surgical risks are reduced by this particularly minimally invasive approach. As there is no risk of damage to bones, muscles and nerves during surgery, this greatly reduces the potential for complications, speeds up the recovery time and improves the overall outcome.
Rehabilitation
Patients may need one day of bed rest and may resume all normal activity within one to six weeks.
Nucleoplasty treatment is, however, only the first step of the long-term solution. Recovery, including pain relief, will be gradual and can take 8-12 weeks to complete. An extensive rehabilitation program will be necessary to ensure the success of the nucleoplasty. Physical activity should be monitored and only gradually increased.
"Back friendly" behaviour such as paying attention to posture, is always advised. It is especially important to strengthen the muscles supporting the vertebral spine and adopt a "back friendly" lifestyle