Treating Morton's neuroma: surgery to save the nerve or remove the nerve?
- Who qualifies for Morton's neuroma surgery?
- Diagnosis and preparing for Morton's neuroma surgery
- How is Morton's neuroma surgery performed at Gelenk-Klinik?
- Orthopaedic surgeon and foot and ankle specialist for Morton's neuroma at Gelenk-Klinik
- Anaesthesia for Morton's neuroma surgery
- Aftercare, rehabilitation following Morton's neuroma surgery
- Should I expect pain after Morton's neuroma surgery?
- How will my treatment be organized at Gelenk-Klinik?
- Important considerations after surgery
- Cost of foot surgery in Germany
- Scheduling your appointment for foot surgery in Germany
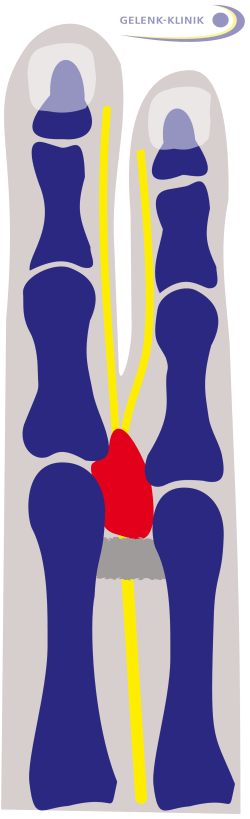 Morton's neuroma (red) as swelling between the metatarsal bones of the toes (blue). If the nerve (yellow) is irritated, burning or stabbing metatarsal pain occurs throughout the area it supplies. © Dr. Thomas Schneider, MD
Morton's neuroma (red) as swelling between the metatarsal bones of the toes (blue). If the nerve (yellow) is irritated, burning or stabbing metatarsal pain occurs throughout the area it supplies. © Dr. Thomas Schneider, MD
Morton's neuroma is a thickening of the metatarsal nerves. It causes acute shooting, burning or stabbing pain in the metatarsus (metatarsalgia) and in the toes. The pain is so severe that patients will only experience temporary relief by sitting down or taking off their shoes. After taking the strain off the foot, the pain quickly subsides. Formication or a feeling of numbness in the toes are symptoms of Morton's neuroma.
Morton's neuroma is a very common result of splayfoot, sometimes in combination with hallux valgus. Women are four times more likely to develop Morton's neuroma than men. This is probably related to footwear: High heels and pointed toes cause a lot of pressure on the front arch of the foot, increasing the risk of developing splayfoot. Splayfoot changes the position of the metatarsal bones and increases pressure on the nerves running along the sole of the foot.
But even men – primarily runners training a lot – can develop it. Morton's neuroma is most likely to occur between the 3rd and 4th toe, and somewhat less likely to occur between the 2nd and 3rd toe.
Who qualifies for Morton's neuroma surgery?
In order to fully assess Morton's neuroma, we need current MRI images. These images are then used to decide together with you if surgery is necessary and what type of surgery is best in your specific case.
In the early stages, Morton's neuroma can often be treated conservatively, using insoles and performing foot exercises. If the personal quality of life has been reduced and pain is severe, and if conservative treatment is unsuccessful, surgery is an option. If the size is less than 0.8 cm, surgery can be used to save the nerve (neurolysis). If Morton's neuroma swelling is too severe, the nerve will need to be removed (neurectomy).
Diagnosis and preparing for Morton's neuroma surgery
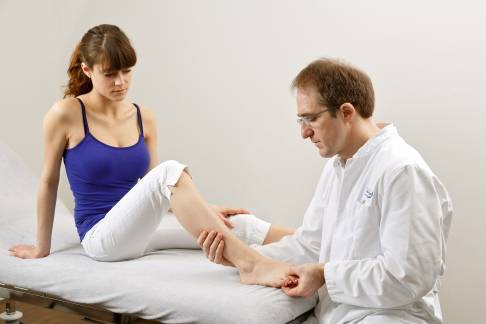 Medical examination for Morton's neuroma using Mulder’s sign: The foot specialist can feel out Morton's neuroma between the metatarsal bones and trigger specific pressure pain. © joint-surgeon
Medical examination for Morton's neuroma using Mulder’s sign: The foot specialist can feel out Morton's neuroma between the metatarsal bones and trigger specific pressure pain. © joint-surgeon
Alternative Causes of Pain in The Forefoot
- Inflammation in any of the joints between the metatarsal bones (bones of the forefoot) and the proximal phalanges (bones at the base of the toe)
- Nerve damage
- Stress fractures in any of the metatarsal bones
- Soft-tissue changes, including scars, warts and tumors
- Improper weight distribution as in the case of pronounced splayfoot
First the physician will perform a thorough diagnostic examination and imaging. Apart from discussing the medical history and a physical examination, this includes MRI images in prone position with contrast agent and in x-rays standing. Podometry (foot pressure measurement) is also helpful to measure the pressure distribution under the bottom of the foot. The physician then uses the results to determine the suitable surgical technique together with the patient.
After determining the patient’s suitability for surgery, the treating physician will discuss the procedure and possible complications of the surgery with the patient. In addition, there will be a discussion with the anaesthetist, who will again review the patient’s health condition with respect to anaesthesia. Once approved by the anaesthetist and the surgeon, the surgery can typically be performed the day after the examination.
How is Morton's neuroma surgery performed at Gelenk-Klinik?
Surgery is reasonable if conservative treatments such as foot orthotics, shoe supply such as butterfly insoles, foot exercises and self-massage or injecting local anaesthetics cannot provide long-term pain relief. There are generallytwo methods which can be used: neurolysis to save the nerve or removing the nerve. Both procedures take about 30 minutes.
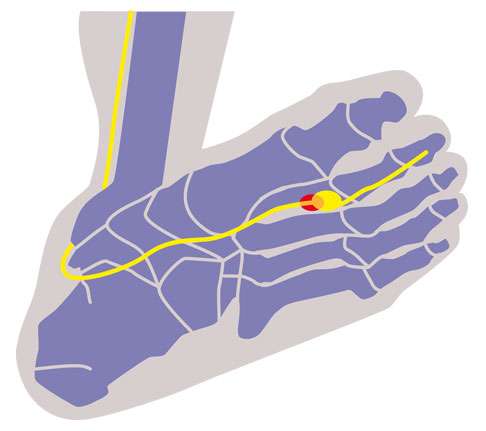 The foot viewed from the sole: In this case, Morton's neuroma is located between the 2nd and 3rd toe. However, it’s more common between the 3rd and 4th toe. © Dr. Thomas Schneider, MD
The foot viewed from the sole: In this case, Morton's neuroma is located between the 2nd and 3rd toe. However, it’s more common between the 3rd and 4th toe. © Dr. Thomas Schneider, MD
Minimally invasive surgery for Morton's neuroma to save the nerve
Nerve compression is caused by mechanical pressure on the plantar nerve of the foot. The irritation of the nerve causes the connective tissue surrounding the foot nerve to swell, scar tissue develops and fluid build.
The swelling causes ischaemia (restriction in supply). The pinching prevents the nerve from being adequately supplied with nutrients. This causes the typical symptoms such as numbness, shooting pain, and tingling. These signs of inflammation are reversible to a certain extent if the mechanical pressure on the nerve is eliminated.
For many nerve compression syndromes (e.g. carpal tunnel syndrome), decompressing the nerve is therefore an appropriate treatment strategy. If the Morton's neuroma is not yet too severe (less than 0.8 cm), it can be operated on just like any other nerve compression syndrome to save the nerve.
We have been seeing excellent medical results for years by relieving the nerve and possibly decompression by repositioning the metatarsal bones. We have particularly seen good results with respect to preventing recurrence (relapse). Recurrences are considerably more likely after amputating the nerve (neurectomy), as this does not remedy the underlying deformity of the arch. Yet neurectomy – so actually amputating the nerve – is still considered the standard treatment for Morton’s neuralgia. All to often the nerve is simply removed (neurectomy) to treat Morton neuralgia without evaluating the procedure to save the nerve.
Benefits of surgery to save the nerve
Endoscopic surgery to save the nerve for Morton's neuroma, accessing from above instead of from below, holds benefits:
- less scarring, thus less irritation to the nerve of the foot after surgery
- lower risk of bruising after surgery
- saving the nerve of the foot, which can be symptom-free (free of pain) and function normally after the nerve sheath swelling has gone down
- lower tendency of recurrence: relapse due to recurrence of painful swelling is common
- lower tendency of developing permanently painful scars around the metatarsal nerve
Neurectomy – removing the inflamed nerve
Neurectomy removes the diseased nerve tissue of the plantar nerve. We also still perform this procedure if the Morton's neuroma swelling is too severe. Here it’s important to determine the size of the Morton's neuroma by MRI. The MRI sectional images, however, do not always definitively provide information on the size and location of the neuroma. The actual surgical strategy is therefore often only determined during the procedure after directly analysing and viewing the Morton's neuroma.
We open the band of connective tissue over the metatarsal head to permanently eliminate pressure on the nerve. This is called decompression. A neurectomy (removing the nerve) is a sound treatment method only if the pressure on the metatarsus is also treated. Otherwise, there is a risk of recurrence, so a renewed irritation of the nerve stump with painful swelling of the connective tissue. Neurectomy is also preferably performed from the top of the foot to avoid scarring in the sole of the foot. This speeds up the healing process and the patient is able to use the foot sooner.
Orthopaedic surgeon and foot and ankle specialist for Morton's neuroma at Gelenk-Klinik
Here at Gelenk-Klinik, a close relationship between the physician and their patient is important. This means: You will be in the care of your treating physician from the initial examination until after surgery. So, you will always have one contact person who will be very familiar with your case and assigned to you throughout your stay at Gelenk-Klinik. Our experts in foot and ankle surgery are the experienced specialists Dr. Thomas Schneider and Dr. Martin Rinio. They’re certified foot and ankle surgeons whose continuing education, diagnostics and surgical quality is reviewed annually by an independent German professional society (DAF). The orthopaedic Gelenk-Klinik is therefore a speciality centre with the title "Centre for foot and ankle surgery" (ZFS).
Anaesthesia for Morton's neuroma surgery
We typically perform Morton’s neuroma surgery under general anaesthesia. However, we also offer spinal anaesthesia to avoid general anaesthesia if the patient so desires. In the case of spinal anaesthesia, an anaesthetist injects the anaesthetic into the spinal canal of the lumbar spine. The patient is fully conscious during surgery. You will decide which type of anaesthesia is best for you together with the anaesthetist. The anaesthetists at Gelenk-Klinik are very experienced in both methods and will choose the option best for the patient and their circumstances based during a pre-operation discussion.
Aftercare, rehabilitation following Morton's neuroma surgery
 After foot surgery, patients are mobile again straight away with the use of a forefoot offloading shoe. This shoe shifts the entire bodyweight to the heel. So patients are also able to travel again. However, you should elevate your foot as much as possible whilst the wound is healing to prevent swelling.
After foot surgery, patients are mobile again straight away with the use of a forefoot offloading shoe. This shoe shifts the entire bodyweight to the heel. So patients are also able to travel again. However, you should elevate your foot as much as possible whilst the wound is healing to prevent swelling.
The inpatient stay after surgery for Morton's neuroma is typically 2 days. After neurolysis you should wear a special shoe to offload the forefoot for 2 to 3 weeks. The foot can bear full weight again about 3 to 6 weeks after neurolysis.
After neurectomy (nerve removal) you will be using the forefoot offloading shoe for about 3 weeks. After that you may wear a normal shoe with a flat sole, which supports the transverse arch and leaves enough room for the toes. In the first 2 months after the operation you should avoid heavier strain and rolling of the foot.
Whilst unable to bear the full weight you will have forearm crutches. Thrombosis prophylaxis (e.g. using Heparin/Enoxaparin) is therefore vital. You should also wear compression stockings until full weight bearing has been restored. We will ensure you receive the aids required after surgery.
Should I expect pain after Morton's neuroma surgery?
Every procedure causes pain. We always strive to keep pain after Morton’s neuroma surgery as low as possible. The assigned anaesthetist will already start pain management during the procedure. In many cases the anaesthetist uses a so-called nerve block during surgery, which keeps the respective foot pain free for approx. 30 hours. This already manages the greatest wave of pain, which can then be easily treated with regular medication. Our goal is for you to experience as little pain as possible after surgery.
How will my treatment be organized at Gelenk-Klinik?
 Private room in the Gelenk-Klinik in Gundelfingen, Germany. © joint-surgeon
Private room in the Gelenk-Klinik in Gundelfingen, Germany. © joint-surgeon
During your inpatient stay at Gelenk-Klinik you will have a single-occupancy room. The room has a bathroom with shower and WC. All rooms include towels, a bath robe and slippers. They further include a mini-bar and safe. All rooms also have a television. You only need to bring your personal medication, comfortable clothes and sleepwear. After surgery you will receive 24-hour care from experienced nursing staff and experienced physiotherapists. The inpatient stay following the procedure is typically 3 days. Your family members can stay at a hotel within walking distance. We will gladly take care of making the reservations.
Important considerations after surgery
Immediately after surgery you should elevate and ice your foot to minimise pain and swelling. The sutures will be removed after about 10 days. At that point you may shower again.
You will also be using a special shoe to offload the forefoot for 2 to 3 weeks. The heel will bear the entire bodyweight. For longer distances, you should also use forearm crutches to relieve your foot. It’s vital to use thrombosis prophylaxis until your foot returns to full weight-bearing. This will prevent dangerous blood clots from forming. You will further receive physiotherapy and lymphatic drainage to prevent muscle loss and minimise swelling of the forefoot. The older the patient, the longer the forefoot will be swollen.
- Inpatient treatment: 2 days
- Optimal local stay: 5–6 days
- Earliest return flight: 3 days after surgery
- Recommended return flight: 5 days after surgery
- Showering permitted: 10 days after surgery
- Recommended time off work: 5 days
- Recommended removal of sutures: 10 days
- Outpatient physiotherapy: 2 weeks
- Time before being able to drive again: 4–5 weeks
- Sports: starting 6 weeks after surgery
Cost of foot surgery in Germany
In addition to the cost of surgery, you will also need to plan for additional costs for diagnostics, physician’s appointments and aids (e.g. forearm crutches). These will cost between 1,500 to 2,000 Euro. If you plan to have outpatient physiotherapy after surgery, we will gladly provide an estimate of costs. You will find information about the cost of hotel lodging and any follow-up treatment at the rehabilitation clinic on the websites of the respective providers.
Scheduling your appointment for foot surgery in Germany
The foot specialists in Germany will first need current MRI images and x-rays of the respective foot to assess the size of the Morton's neuroma and possibly other foot conditions. After sending these documents to us through our website, we will send you patient information including proposed treatment and a binding estimate of costs within 1–2 days.
Gelenk-Klinik offers quick appointments for international patients to correspond with your preferred travel itinerary. We will gladly help you apply for a visa once we have received the down payment specified in the cost estimate. If the visa is denied, we will promptly refund the full down payment by remittance.
We try to minimise the time between the preliminary examination and the surgery for our international patients to avoid additional travel. During your inpatient and outpatient stay our multi-lingual (English, Russian, Spanish, Portuguese) case management team will be there to assist you. We can also provide an interpreter (e.g. Arabic) at any time, at the patient’s expense. We will gladly assist you with organising transportation and lodging and provide tips for recreational activities for your family members.