Herniated Disc in the Lower Back (Lumbar Disc Herniation)
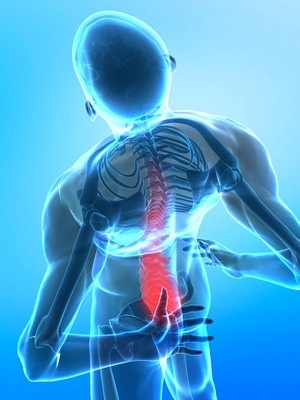 Expert Diagnosis of Lumbar Spine Disorders © Viewmedica
Expert Diagnosis of Lumbar Spine Disorders © Viewmedica
Vertebral discs are usually only mentioned in connection with herniated discs and back pain: our spinal discs tend to have a bad reputation. Most people start to consider the existence of vertebral discs only after a painful discus prolapse causes extreme pain. Other symptoms such as tingling, numbness and weak reflexes indicate loss of nerve function in the spine.
Spinal Discs keep the Vertebral Column Flexible
We frequently hear stories of people having problems with their discs. But it is important to remember that our discs have a vital function: We have 23 Spinal discs. The spinal column is made up of a rather hard and stiff series of bone blocks (vertebrae) and tight ligaments. With the soft spinal disc, the spine gets a remarkable degree of flexibility. Spinal discs therefore, make an essential contribution to our capacity to move around easily.
Biomechanics of Spinal Discs: Flexibility and Shock Absorption
In addition to securing basic flexibility, our spinal discs act as shock absorbers. Spinal discs are also capable of distributing and effectively absorbing shearing and stress forces. When we move about and carry a load, the stress is many times greater than our body weight. This shock-absorbing quality is made possible by the simple structure of spinal discs. They consist of a gelatinous core (known as the nucleus pulposus). The soft core is surrounded by a hard ring of fibrocartilage and fibrous tissue (known as the annulus).
The Life Cycle of the Vertebral Disc
The biomechanical properties of our discs change throughout the day: spinal discs lose water and height during the day and expand during the night.
Spinal discs also change during our lifetime. Spinal discs start ageing from the moment we are born. Our spinal discs undergo a degenerative process that is more extensive than that seen in any other type of tissue. During the embryonic phase, our discs are supplied with nutrients by their own blood vessels.
After birth the supply of water and nutrients in adults takes place exclusively via diffusion. Movement helps to keep the spinal disc’s metabolism intact and slows down the ageing process. Conversely, immobility and a sedentary lifestyle accelerate the degeneration of spinal discs.
Our discs contract during the day as they carry the weight of our bodies. They expand like a sponge at night, as they take in water in their unloaded state. The difference in the size of our discs in the morning and evening may vary by several centimetres. As we age, the gelatinous core of our discs gradually shrinks. This brings about changes in the overall structure of the biomechanical property of the disc.
Disc herniation
Exposed to additional stress, the fibre ring (annulus) may bulge outwards (just as a rubber ball does if we squash it between our hands) and begin to exhibit tears and fissures. This "bulging" of the annulus commonly leads to spinal disc herniation. Spinal disc herniation occurs when a portion of the gelatinous core pushes out beyond the boundary of the fibre ring. The gelatinous core can protrude into the spinal canal and damage the spinal nerves running through this area.
Back Pain Associated with Disc Protrusion and Herniation
The protrusion of the disc or the extrusion (leaking) of disc material into the spinal canal can pinch highly sensitive nerve roots. This process can cause considerable pain both at the point of impact and in the areas of the body (e.g. the legs) that are served by those nerves.
In addition to this, sensory and functional problems, including numbness, tingling and loss of muscle strength, may occur. The extent of these problems depends on the degree to which the nerve pathways (carrying signals to and from our brains), are compromised.
The extrusion of the gelatinous material that is normally contained within the annulus leads to sensory and functional problems, more frequently than mere disc protrusion (bulging).
Moreover, the disc material that leaks into the spinal canal (either in the direction of the head or the feet) may become detached. This peculiarity is known as sequestered herniation and can cause nerve root irritation at a point far away from the damaged disc.
It is important to be aware, however, that some people may experience no symptoms whatsoever when disc herniation occurs. Investigations of the affected nerve tissue in such cases suggest that an adaptive process can take place, whereby the pain receptors in the affected tissue recede. This emphasizes the importance of using infiltration therapy to confirm or rule out the need for disc surgery.
Diagnosing Disc Herniation
The task of diagnosing disc herniation should only be performed by a specialist by thorough examination which involves consultation with specialists in other, related fields of medicine.
An MRI or a CAT scan can serve to support a diagnosis and determine which disc is involved. Contrast media may also be used in the visualization of the disc and the spinal canal.
Surgery should not be performed for disc herniations that can only be detected using MRI and produce no symptoms.
Treatment for Herniated Discs
Treatment for herniated discs generally focuses on removing or reducing the extruded disc material so as to relieve the pinched nerve root. Several minimally invasive procedures may be used depending on the location and extent of the herniation or protrusion involved.
These include nucleoplasty, Racz catheter treatment, disc-FX treatment, endoscopic disc removal, disc replacement and open microsurgical removal of extruded material.
Given that most herniated discs do respond favourably to conservative forms of treatment, it is important to exercise caution when considering surgery. On the other hand, it may be necessary in the case of disc herniations that lead to functional disturbances (such as a loss of muscle strength and lameness), to remove the extruded disc material as quickly as possible, so as to prevent irreversible damage to the affected nerves.