Shoulder Pain: causes and therapy
- What are the causes of shoulder pain?
- When is surgery a good option for shoulder pain?
- How is shoulder surgery performed in Gelenk-Klinik?
- Your shoulder specialist: Which doctors specialise in shoulder surgery?
- Preparing for shoulder surgery
- What type of anaesthesia is used for shoulder surgery?
- Which aids will I need following shoulder surgery?
- Should I expect pain after shoulder surgery?
- What will my stay be like for the shoulder surgery?
- What do I need to keep in mind after surgery?
- What is the cost of shoulder surgery?
- How can international patients schedule shoulder surgery?
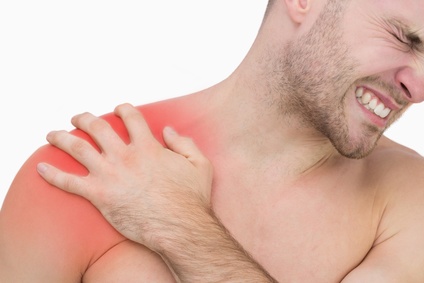 Almost one in ten patients complains of shoulder pain. © WavebreakmediaMicro, Fotolia
Almost one in ten patients complains of shoulder pain. © WavebreakmediaMicro, Fotolia
Shoulder pain can have many different causes. Muscle tension is common. But also traumata, arthrosis, calcifications or inflammations can cause pain in the highly complex shoulder joint. The structures affected are not only muscles: Tendons, ligaments and bones may also be affected. The prevalence of both acute and chronic shoulder pain has increased significantly among the general population over the last few years.
Almost every tenth patient suffers from shoulder pain today. This is due to the demographic development of the age groups, but increasingly also can be traced back to today’s tendency to lead a sedentary lifestyle and to hunched shoulders.
Shoulder problems often cause excruciating pain that severely restricts mobility and persists over a long period of time. Pain at night can be particularly unpleasant. After injuries or inflammations of the shoulder joint, patients are often unable to lie on the affected shoulder for weeks. The pain can be both sharp and dull in nature.
What are the causes of shoulder pain?
Acromioclavicular joint separation (AC separation)
The acromioclavicular joint - also known as the AC joint - is the articulated joint between the acromion and the outer end of the collarbone (clavicle). It is the highest point of the shoulder.
The AC joint allows the arm to be raised above head height and when injured, the arm can no longer be lifted to this height. AC joint injury is a typical sport injury in cyclists, gymnasts or those that play ball sports. In most cases, a fall onto the shoulder is the cause of the injury.
The character of the injury can be very varied. The ligament connections between the acromion and collarbone (clavicle) may be affected, depending on the severity of the trauma. Similarly, the ligaments between the clavicle and the coracoid process, an extension of the shoulder blade, can tear.
Labral tear: Tearing of the glenoid labrum
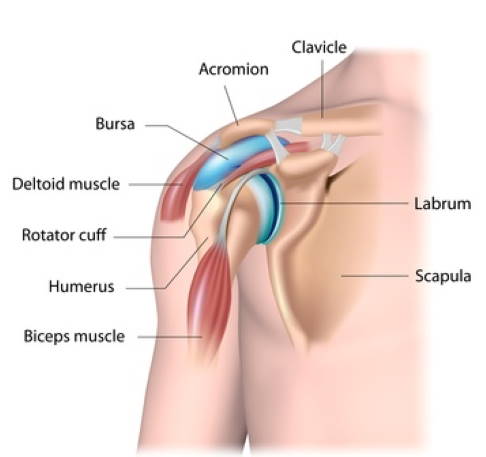
The glenoid labrum (labrum glenoidale) is a cartilaginous, connective tissue surrounding the socket (glenoid) of the shoulder joint. The labrum plays a major role in guiding and aligning the humeral head with the shoulder joint. It surrounds the humeral head, enlarges the surface area of the joint and therefore supports joint stability and the nutrition of the cartilage.
If the labrum becomes damaged after a trauma, fall or a dislocation of the shoulder, the shoulder joint becomes unstable. Damage to the glenoidal labrum results in shoulder pain in the underarm region. Over the long term, it is not only the exertion of strength that is inhibited, a labral tear can also lead to shoulder arthrosis (omarthrosis).
Rupture of the rotator cuff and the supraspinatus tendon
The rotator cuff is a ring of muscles and tendons. This ring ensures that the healthy shoulder joint is able to deliver the strength required in almost every direction. If one of the rotator cuff tendons (e.g. the strong supraspinatus tendon) is damaged or torn, some movements become painful and the supporting muscles degenerate. Generally, the acute (accident-related) rupture after a fall on the elbow can be clearly distinguished from chronic deterioration of the rotator cuff. In many cases, the chronic condition occurs later in life or as a result of postural problems caused by an impingement syndrome (shoulder impingement).
A focus of attention in this respect is often placed on the rotator cuff’s supraspinatus tendon, which runs from under the acromion and extends over the humeral head. This is the tendon most frequently affected by defects. The supraspinatus tendon plays a crucial role in the transmission of force required to raise the arm.
 The rotator cuff has a strong supraspinatus tendon that surrounds the humeral head from above and centres it in the shoulder joint. © Alila Medical Media, Fotolia
The rotator cuff has a strong supraspinatus tendon that surrounds the humeral head from above and centres it in the shoulder joint. © Alila Medical Media, Fotolia
Shoulder impingement
Shoulder impingement is a narrowing of the structures under the acromion. Contact between the humerus and the acromion often occurs when the arm is extended outwards. This movement can cause muscles and tendons to get caught between the bones. The supraspinatus tendon of the rotator cuff is particularly affected by this. The tendon degenerates and may eventually tear, even under minimal strain. A tear in the supraspinatus tendon further increases the severity of the narrowing under the acromion. Without the resistance from the tendon, the muscular tension pulls the upper arm upwards toward the acromion.
Impingement syndrome particularly causes shoulder pain under strain. Handball players, volleyball players, tennis players, but also those predominantly working overhead such as painters or industrial workers, place considerable strain on their shoulders due to the force exerted in this extreme extended position. This often leads to the typical shoulder pain associated with shoulder impingement syndrome.
The pain may radiate from the shoulder into the arm. Extending the arm at range of 60°-90° degrees, i.e. horizontally, is a particularly painful motion. This range is known as the ‘painful arc’.
 With shoulder impingement, extending the arm - especially at an angle of 60°-90° - is painful. © joint-surgeon
With shoulder impingement, extending the arm - especially at an angle of 60°-90° - is painful. © joint-surgeon
Biceps tendon tear
Supraspinatus tendon disorders are often accompanied by inflammation or even rupture of the biceps tendon. A shoulder impingement also puts pressure on the biceps tendon. This results in it being permanently compressed and can cause painful inflammation.
If the biceps tendon is just somewhat sore, we speak of tendinitis of the biceps tendon. A typical test of biceps tendon function is to bend the arm at the elbow whilst resistance is applied. The physician can trigger this typical shoulder pain by applying pressure to the front region of the rotator cuff. If the biceps tendon is subject to prolonged wear and tear, a rupture may also occur. A typical thickening of the biceps muscle's deep-seated muscle belly develops after a tendon tear.
Shoulder arthrosis (omarthrosis)
Shoulder arthrosis (omarthrosis) is the progressive wear of the joint surfaces of the shoulder joint accompanied by cartilage loss, painful stiffening and diminishing strength.
Just like in any other joint, cartilaginous surfaces keep the shoulder joint flexible and free-moving. Shoulder arthrosis typically causes dull and deep pain in the shoulder. The pain can increase when throwing or when working overhead, for example.
When the shoulder joint cartilage is damaged due to inflammation, an accident or degeneration, the shoulder becomes increasingly stiff and painful. Typical shoulder arthrosis pain can be felt in the underarm. In contrast to the weight-bearing joints of the lower extremities (hip arthrosis, knee arthrosis, ankle arthrosis), the shoulder is rarely affected by arthrosis.
 With shoulder arthrosis, extending the arm - especially at an angle of 90°-120° - is painful. © joint-surgeon
With shoulder arthrosis, extending the arm - especially at an angle of 90°-120° - is painful. © joint-surgeon
Calcific tendinitis
Calcific tendinitis (tendinosis calcarea) is a disorder of the shoulder tendons, in particular the supraspinatus tendon. The cause is considered to be insufficient blood circulation in the rotator cuff, causing calcium deposits. Therefore, the degree of strain on the shoulder as well as previously sustained injuries or falls on the shoulder do not appear to be relevant. The majority of patients affected are between 40 and 50 years old.
Bursitis of the shoulder (inflammation of the bursa)
The bursa is a sliding buffer tissue filled with lubricating synovial fluid. It can be found wherever different tissues and movement systems need to be moved flexibly and frictionlessly against each other. These are muscles, tendons and bones.
The largest of the body's synovial bursa is the bursa subacromialis. Inflammation of this bursa in the shoulder is one of the most common causes of acute shoulder pain. In most cases, this is preceded by excessive strain, for example due to working overhead. This can lead to the emergence of micro-injuries and crystals, which then trigger an aseptic (bacteria-free) inflammation. In isolated cases, the crystallisation of e.g. uric acid (gout) can also occur as a result of a change in eating habits, diets, etc.
Frozen shoulder (adhesive capsulitis)
Frozen shoulder or adhesive capsulitis of shoulder, is a painful, non-bacterial inflammation of the shoulder's joint capsule. This causes the joint capsule of the shoulder joint to shrink and stick together. This results in severe, often painful reduction in shoulder mobility (primary frozen shoulder). Primary frozen shoulder has a variety of causes and is therefore still not entirely clear.
Stiffness in the shoulder can also arise as a result of illness or injury. This is referred to as a secondary frozen shoulder. Following an inflammatory acute phase, the shoulder often remains immobile for a period of more than six months. Metabolic diseases like diabetes and thyroid disorders tend to exacerbate frozen shoulder.
When is surgery a good option for shoulder pain?
In some cases, even more conservative methods (physiotherapy, injections, shock wave therapy) can bring about a significant improvement in shoulder pain. However, if considerably limited mobility and stiffness are evident, surgical intervention is recommended. In addition, any structural damage to ligaments and tendons in ultrasound or MRI images often require surgery. Degenerative conditions (arthrosis) and inflammations (e.g. bursitis) as well as persistent, severe pain frequently require surgery if pain can no longer be managed with conservative treatment.
How is shoulder surgery performed in Gelenk-Klinik?
When exactly shoulder pain requires a surgery depends on the precise diagnosis of the shoulder specialist and the progression of the disorder. At Gelenk-Klinik, we offer all open and minimally invasive (arthroscopic) surgical procedures to treat shoulder disorders. With open surgery, the physician exposes the area through a long skin incision and can see it completely.
Arthroscopic shoulder surgery only requires skin incisions 0.5-1 cm in length. The surgeon can insert slim tubes only a few millimetres in diameter into the joint through these incisions. The tubes allow optics and small surgical instruments to be inserted into the shoulder joint and then moved along to any tendons, bones and cartilage without the need for any further incisions. Arthroscopic shoulder surgery is always our preferred method: It is less painful and heals quickly.
This is why the majority of shoulder procedures we perform at Gelenk-Klinik are arthroscopic. Our shoulder specialists have the experience to even make complex tendon sutures, perform bursectomies, mucosectomies, or to remove calcium deposits arthroscopically.
The greatest benefit of arthroscopy is that it requires no large incisions in the skin, soft tissues and other tissues to reach the surgical site. A monitor displays a direct view of the surgical site captured by the small camera at the end of the flexible tube.
Compared to open surgery, this results in considerably less injury and scarring which could later in turn cause shoulder pain. Even the risk of post-surgical complications is greatly reduced due to the smaller scar and quicker healing. The patient can start exercising the shoulder slightly the day after arthroscopy.
Your shoulder specialist: Which doctors specialise in shoulder surgery?
Here at Gelenk-Klinik we believe a close relationship between the physician and their patient is important. This means that you will be in the care of your shoulder specialist from discussing your medical history until after surgery. So you will have one doctor, who will be very familiar with your condition and assigned to you throughout your stay at Gelenk-Klinik. Our specialists for shoulder pain and shoulder arthroscopy are Dr. Marquaß and Dr. Ostermeier.
Preparing for shoulder surgery
First the physician will perform a thorough medical examination of the shoulder. Diagnostic imaging is used to help analyse the results. Medical examination means: Discussing your medical history and a physical examination including testing the mobility of the shoulder joint. Diagnostic imaging means: Taking x-rays to assess the condition of the bones. In addition, an MRI (magnetic resonance imaging) and ultrasound are important to determine any damage to the muscles, tendons and bursae.
After determining the patient’s suitability for surgery, the treating physician will discuss the procedure and possible complications of shoulder surgery with the patient. In addition, there will be a detailed discussion with the anaesthetist, who will again review the patient’s health condition with respect to anaesthesia. Once approved by the anaesthetist and the surgeon, the surgery can typically be performed the day after the examination.
 Diagnostic imaging (ultrasound) helps the shoulder specialist detect damage to muscles, tendons or bursae. © joint-surgeon
Diagnostic imaging (ultrasound) helps the shoulder specialist detect damage to muscles, tendons or bursae. © joint-surgeon
What type of anaesthesia is used for shoulder surgery?
Shoulder surgery is performed under general anaesthesia. The anaesthetist will inject a combination of anaesthetics tailored to your body. You will feel no pain during the surgery and will not be aware of the procedure. An experienced anaesthetist will be present throughout the procedure, monitoring your vital functions and ensuring you do not wake up during the surgery.
Which aids will I need following shoulder surgery?
 With some injuries, such as acromioclavicular separation, the shoulder is immobilised with a Gilchrist bandage. © Dan Race, Fotolia
With some injuries, such as acromioclavicular separation, the shoulder is immobilised with a Gilchrist bandage. © Dan Race, Fotolia
In the first days following surgery it will be important to rest your shoulder. To ensure this, you will receive a shoulder brace, meaning a support bandage, which stabilises the shoulder. Some injuries such as a torn rotator cuff require the shoulder joint be kept at a specific angle. This can be achieved through use of an abduction splint or an abduction cushion.
Should I expect pain after shoulder surgery?
Every procedure causes pain. We always strive to keep pain after shoulder surgery as low as possible. You will typically receive a nerve block, which numbs the respective extremity for about 30 hours. This already manages the greatest wave of pain, which can then be easily treated with regular medication. Our goal is for you to experience as little pain as possible after shoulder surgery.
What will my stay be like for the shoulder surgery?
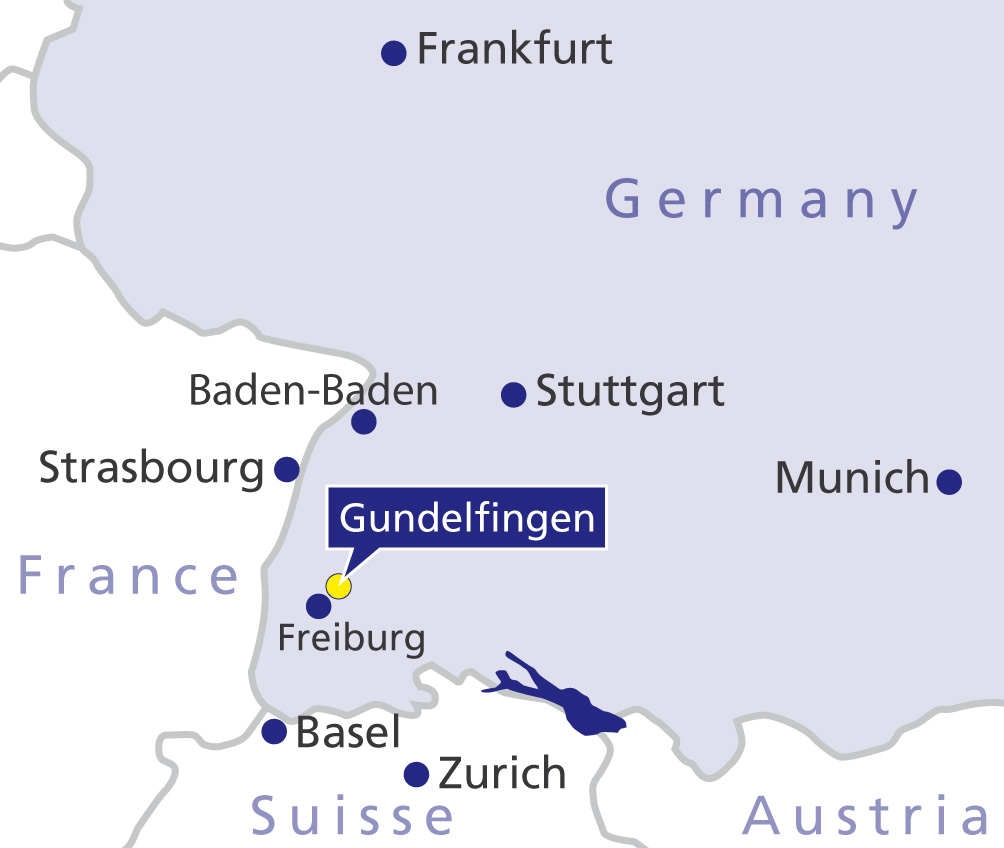
 Private room in the Gelenk-Klinik in Gundelfingen, Germany
Private room in the Gelenk-Klinik in Gundelfingen, Germany
During your inpatient stay at Gelenk-Klinik you will have a single-occupancy room. The room has a bathroom with shower and WC. All rooms include towels, a bath robe and slippers. They further include a mini-bar and safe. All rooms also have a television. You only need to bring your personal medication, comfortable clothes and sleepwear. After surgery you will receive 24-hour care from experienced nursing staff and experienced physiotherapists. The inpatient stay following shoulder surgery is typically 3 days. Your family members can stay at a hotel within walking distance. We will gladly take care of the reservation and planning your stay for you.
What do I need to keep in mind after surgery?
After surgery you should rest your shoulder and avoid any sudden movement. Your shoulder will be placed in an appropriate brace for 6 weeks. This will only allow minimal external and internal rotation exercises and passive mobilisation. You should refrain from active training and building muscle until 6 weeks after the surgery. Depending on the physician’s instructions you will receive manual therapy to resolve functional disorders of the musculoskeletal system from our experienced physiotherapists. The stitches will be removed between the 5th and 7th day post-op. Showers are permitted 7 days after the operation.
- Inpatient treatment: 3 days
- Optimal local stay: 10 days
- Earliest return flight: 7 days after surgery
- Recommended return flight: 10 days after surgery
- Showering permitted: 7 days after surgery Recommended time off work: 6 weeks (varies by job)
- Recommended removal of sutures: 5 to 7 days
- Time before being able to drive again: 6-8 weeks
- Outpatient physiotherapy: 2 weeks
What is the cost of shoulder surgery?
In addition to the cost of shoulder surgery you will also need to plan for additional costs for diagnosis, physician’s appointments and aids (e.g. shoulder brace). If you plan to have the outpatient physiotherapy in Germany after surgery, we will gladly schedule the appointments with the physiotherapists and obtain an estimate of costs. You will find information about the cost of hotel lodging and any follow-up treatment at the rehabilitation clinic on the websites of the respective providers. We will gladly assist you with planning your rehabilitation stay.
How can international patients schedule shoulder surgery?
We will first need recent MRI images, and particularly x-rays of the shoulder to assess the condition of the bones and the joint. After sending these to us through our website, we will send you patient information including proposed treatment and a binding estimate of costs within 1–2 days.
Gelenk-Klinik offers quick appointments for international patients to correspond with your preferred travel itinerary. We will gladly help you apply for a visa once we have received the down-payment specified in the cost estimate. If the visa is denied, we will promptly refund the full down-payment.
We try to minimise the time between the preliminary examination and the surgery for our international patients to shorten your stay and avoid additional travel. During your inpatient and outpatient stay our multi-lingual (English, Russian, Spanish, Portuguese) case management team will be there to assist you. We can also provide an interpreter (e.g. Arabic) at any time, at the patient’s expense. We will gladly assist you with organising transportation and lodging and provide tips for recreational activities for your family members.