Cruciate ligament tear: Surgery, rehabilitation, costs
- Cause and progression of a cruciate ligament tear
- When does a cruciate ligament tear require surgery?
- What happens before surgery for a torn cruciate ligament?
- How is cruciate ligament surgery performed at Gelenk-Klinik?
- Which type of physician operates on a torn cruciate ligament?
- Success rates after cruciate ligament surgery
- What type of anaesthesia is used for cruciate ligament surgery?
- After-care, rehabilitation and aids following cruciate ligament surgery
- Should I expect pain after cruciate ligament surgery?
- What will my stay be like at Gelenk-Klinik?
- What do I need to keep in mind after cruciate ligament surgery?
- How much is knee surgery?
- How can international patients schedule cruciate ligament surgery?
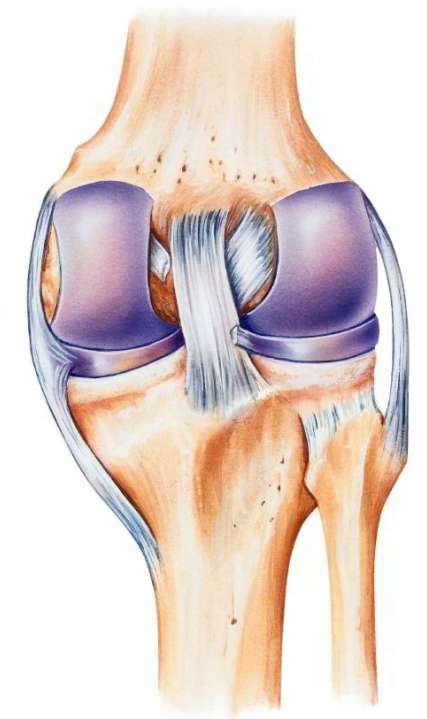 The anterior and posterior cruciate ligament are located at the middle of the knee. The cartilage surfaces and the menisci on the tibial end are identified in purple. The cruciate ligament can easily be stretched or injured due to twisting (distortion) or impact on the knee. When it is ruptured, we refer to a cruciate ligament tear. © Istockphoto.com/MedicalArtInc
The anterior and posterior cruciate ligament are located at the middle of the knee. The cartilage surfaces and the menisci on the tibial end are identified in purple. The cruciate ligament can easily be stretched or injured due to twisting (distortion) or impact on the knee. When it is ruptured, we refer to a cruciate ligament tear. © Istockphoto.com/MedicalArtInc
At the middle of the knee are two crossing ligaments which connect the thigh (femur) and shin (tibia) and keep them in place. A rupture (tear) of one or two cruciate ligaments makes the knee unstable. A cruciate ligament tear is most common in the anterior cruciate ligament. It is often caused by sports injuries just as twisting (distortion) of the knee whilst skiing or a collision during ball games.
A torn cruciate ligament will cause severe swelling of the knee and stabbing pain. Often, a crack or pop can be heard when the cruciate ligament tears and the person feels a jerk in the knee. The patient is unable to move the knee to the full extent. To stabilise the knee and prevent knee arthrosis, the orthopaedist can either sew the cruciate ligament or replace it with a ligament transplant.
Cause and progression of a cruciate ligament tear
An anterior cruciate ligament tear is typically a sports injury. In many cases, the lower leg twists away from the mechanical axis of the leg (distortion). The following situations are typical for this type of injury:
- an opponent in football hitting the side of the knee hard
- overextending the knee
- stopping abruptly whilst running at full speed
- suddenly changing directions whilst running at full speed
- unfortunate landing after jumping or turning
A typical situation is e.g. an opposing player in football tackling the leg. A cruciate ligament tear is also quite common in skiing when falling and twisting or overextending the lower leg.
The patient typically feels a tear in the knee at the time of the accident. The cruciate ligament tear is often accompanied by an audible pop from the overextended and tearing ligament. A cruciate ligament tear requires considerable force to be placed on the ligament. The cruciate ligament has a breaking strength of about 2400 kg. However, its tear strength varies: In women, the diameter is smaller, so they are more likely to suffer from a cruciate ligament tear. In children, the cruciate ligament often tears out of the anchor in the tibia (shin).
A tear of the posterior cruciate ligament requires substantially greater force than an anterior cruciate ligament tear. It is considerably stronger. A strain of this magnitude is common in traffic accidents, for example when the knee hits the interior of the car. Injuries to the posterior cruciate ligament are therefore much rarer. Only about 7–10% of cruciate ligament tears affect the posterior cruciate ligament.
When does a cruciate ligament tear require surgery?
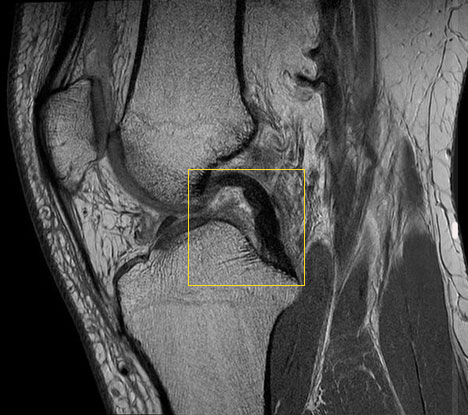 The intact posterior cruciate ligament runs from the front of the thigh to the posterior surface of the shin. © Radiopedia.org
The intact posterior cruciate ligament runs from the front of the thigh to the posterior surface of the shin. © Radiopedia.org
 Same patient: The anterior cruciate ligament cannot be identified, as it was damaged by a cruciate ligament tear. © Radiopedia.org
Same patient: The anterior cruciate ligament cannot be identified, as it was damaged by a cruciate ligament tear. © Radiopedia.org
If conservative treatment options do not yield good results and the patient is young and very active, surgical reconstruction of the cruciate ligament is sensible to maintain the quality of life and sporting activity. Furthermore, a rupture of over 75 % of the cruciate ligament or avulsion from the bone requires surgery.
If the cruciate ligament tear is left untreated, the knee will suffer subsequent damage over the years. The joint surfaces and the menisci will be subjected to excessive strain. There is a risk of premature cartilage wear, cartilage damage, and after 10–15 years, arthrosis of the knee joint. The remaining instability of the knee following a cruciate ligament tear will often also result in a torn meniscus.
In about 80 % of cases, a cruciate ligament tear will damage other structures in the knee:
- Medial meniscus tear (69 % probability)
- Lateral meniscus tear (49 % probability)
- Cartilage damage (20–50 % probability)
- Secondary knee arthrosis due to limited meniscus function
- Medial collateral ligament injury (common)
- Lateral collateral ligament injury (less common)
- Tear of the knee capsule
What happens before surgery for a torn cruciate ligament?
Prior to surgery, the physician will conduct detailed medical diagnostics. He will first ask the patient about the accident and any remaining feelings of instability. This provides information about the type and extent of the cruciate ligament injury. Unfortunately, a cruciate ligament tear is often only diagnosed years later, since many patients consider the accident a trivial injury ("sprain").
If the patient has strong thighs, a cruciate ligament injury is often not medically diagnosed and the trauma is initially overcome without further treatment. However, over the course of time, the instability worsens. Arthrosis can develop, as the accident often also damages the cartilage inside the knee. The problems are often not discovered for years. Instability arises, e.g. when walking upstairs or with rotary motion. The result is persistent knee pain.
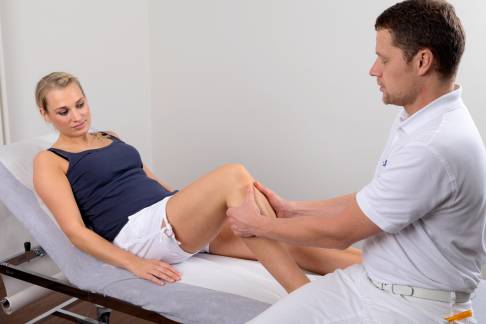
In addition to testing movement, which is most likely to shed light on concomitant meniscus injuries, specific stability tests (drawer test, Lachman test, pivot-shift test) can be used to diagnose a cruciate ligament tear.
 The cruciate ligament function can be determined with the Lachman test. The test is similar to the drawer test but performed with the knee bent 30°. © joint-surgeon
The cruciate ligament function can be determined with the Lachman test. The test is similar to the drawer test but performed with the knee bent 30°. © joint-surgeon
In addition, MRI imaging can easily show the torn cruciate ligament. An X-ray is necessary to rule out concomitant damage to the bone in the knee. Joint aspiration – extracting synovial fluid from the knee complex – can provide information about a cruciate ligament tear: Since the cruciate ligaments are well supplied with blood, the rupture of the cruciate ligament causes bleeding into the joint. Blood is detected in the synovial fluid.
After the diagnosis has been made and the patient has been deemed fit for surgery, the treating physician will discuss the procedure and possible complications of surgery with the patient. In addition, there will be a discussion with the anaesthetist, who will again review the patient’s health condition with respect to anaesthesia. Once approved by the anaesthetist and the surgeon, the surgery can typically be performed the day after the examination.
How is cruciate ligament surgery performed at Gelenk-Klinik?
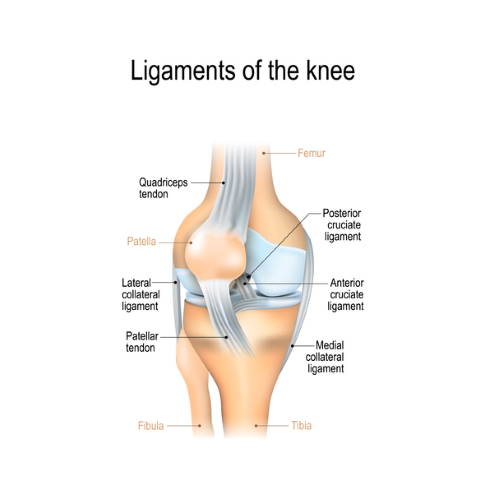 The lateral or medial ligaments of the knee can spontaneously grow together. This self-healing process does not occur in the anterior and posterior cruciate ligament. © ttsz, iStock
The lateral or medial ligaments of the knee can spontaneously grow together. This self-healing process does not occur in the anterior and posterior cruciate ligament. © ttsz, iStock
Acute injury following a cruciate ligament tear has consequences: After a rupture, the cruciate ligament can only be operated on once the wound and all associated injuries have healed. Cruciate ligament reconstructions is therefore performed about two to three months after the cruciate ligament tear. During this time, knee function is considerably limited. Concomitant physiotherapy can prepare the knee for surgery in this period.
The cruciate ligament is unlike other ligaments in the knee: If the lateral or medial ligaments of the knee are torn, immobilising the joint with braces can typically allow them to spontaneously grow together. This self-healing process does not occur in the anterior and posterior cruciate ligament. Surgery of the cruciate ligament is typically required to restore cruciate ligament function.
The surgery to repair a cruciate ligament tear takes about 1.5 to 2 hours. Two different techniques can be used: the tendon transplant and cruciate ligament suture. Which procedure is suitable in your specific case needs to be discussed with your treating physician.
Cruciate ligament reconstruction by tendon transplant
The traditionally most commonly used surgery is cruciate ligament reconstruction. The surgeon first removes the entire torn cruciate ligament to prepare for cruciate ligament reconstruction. Parts of other tendons in another location of the knee are removed to use as the graft. Typically, part of the patellar tendon between the patella and tibia is used. But even the hamstring, located at the back of the knee, can be used as the body’s own (autologous) transplant.
The advantage of an autologous graft is that the body obviously will not reject the transplant. The graft is harvested from the patient’s body – patella tendon or hamstring tendon. After anchoring it to the femur and tibia with bone screws, the body soon assimilates it and supplies it with blood vessels which grow into the graft.
One drawback of the autologous tendon transplant to treat the cruciate ligament tear is the painful weakening of the leg caused by harvesting the tendon (so-called harvesting pathology). The areas where the tendon is harvested are sometimes painful and weak for months. Harvesting the tendon reduces the maximum strength. However, this is only important in competitive athletes. Following surgery, the patient will require a lot of physiotherapies and rehabilitative training.
Cruciate ligament reconstruction, however, also does not restore the nerve supply of the cruciate ligament crucial for coordination. This can also have its drawbacks in competitive sports. However, in most patients this is irrelevant.
Cruciate ligament sutures by reaffixing the torn cruciate ligament
A modern treatment option can maintain the body’s cruciate ligament following a cruciate ligament tear. The implant system used has only been available since early 2014. With the help of this system, the torn cruciate ligament is initially stabilised with an artificial implant. During the healing phase, it mechanically stabilises the torn cruciate ligament in the centre of the knee joint. The torn stubs are fused back together and can heal, protected by the implant. If successful, cruciate ligament reconstruction using the body’s own tendons is no longer necessary.
The outcome of implant refixation of the cruciate ligament is better than with an autologous tendon graft, as this procedure completely preserves all nerves in the cruciate ligament and thus the motor control of all reflexes of the knee. This can be crucial for athletes.
A graft does not need to be harvested from the body to refix the tendon. This means that there is no harvest pathology involving pain and muscle weakness at the harvest site. The patient will have full use of the torn cruciate ligament just days after the refixation.
A detailed MRI is required before a decision can be made on surgical refixation of the cruciate ligament. The procedure is very time-critical: After more than three weeks following the trauma, the torn cruciate ligament is no longer able to regenerate quite so well. So refixation requires surgery during the acute phase within the first three weeks following the cruciate ligament tear. After that, the only option is a cruciate ligament transplant.
We can remove the temporary implant after successful healing of the torn cruciate ligament about six to nine months after the operation in a small surgical procedure. When the implant is removed, we check arthroscopically how the cruciate ligament has healed.
Which type of physician operates on a torn cruciate ligament?
Here at Gelenk-Klinik we believe a close relationship between the physician and their patient is important. Meaning, you will be in the care of your treating physician from the initial appointment until after the cruciate ligament surgery. This physician is also responsible for your aftercare. So, you will have one contact person who will be assigned to you throughout your stay at Gelenk-Klinik. Our knee specialists are Prof. Dr. Ostermeier and PD Dr. Marquaß.
Success rates after cruciate ligament surgery
Cruciate ligament surgery is a very successful surgery which restores the function of the knee in over 90 % of cases. Most patients can return to competing in sports or to work following cruciate ligament surgery. Cruciate ligament surgery is a common surgery, meaning that we are very experienced in this procedure.
What type of anaesthesia is used for cruciate ligament surgery?
Cruciate ligament surgery is typically performed under general anaesthesia. However, we also offer spinal anaesthesia to avoid the risks of general anaesthesia. In the case of spinal anaesthesia, an anaesthetist injects the anaesthetic into the spinal canal of the lumbar spine. The patient is fully conscious during surgery. Our anaesthetists are very experienced in both methods and choose the option best for you and your circumstances during a mutual pre-operation discussion.
After-care, rehabilitation and aids following cruciate ligament surgery
During the first few days after surgery, the knee will be immobilised in a straight knee brace (Mecron brace) at 0° flexion. We then use a 4-point stabilisation, in which the flexion and extension of the knee joint can be individually adjusted. You will further receive forearm crutches to reduce strain on the knee. Thrombosis prophylaxis (e.g. Heparin/Enoxaparin) is vital during this time. You should further use compression socks until full weight bearing has been restored. We will ensure you receive the aid required after surgery.
Should I expect pain after cruciate ligament surgery?
Every procedure causes pain. We always strive to minimise pain as much as possible. The anaesthetist often uses a so-called nerve block before the surgery, numbing the respective knee for about 30 hours. This already manages the greatest wave of pain, which can then be easily treated with regular medication. Our goal is for you to experience as little pain as possible.
What will my stay be like at Gelenk-Klinik?
 Private room in the Gelenk-Klinik in Gundelfingen, Germany. © joint-surgeon
Private room in the Gelenk-Klinik in Gundelfingen, Germany. © joint-surgeon
During your inpatient stay at Gelenk-Klinik you will have a single-occupancy room. The room has a bathroom with a shower and WC. All rooms include towels, a bathrobe and slippers. They further include a mini-bar and a safe. All rooms also have a television. You only need to bring your personal medication, comfortable clothes and sleepwear. After surgery you will receive 24-hour care from experienced nursing staff and experienced physiotherapists. The inpatient stay following the procedure is typically 3 days. Your family members can stay at a hotel within walking distance. We will gladly take care of making the reservations.
What do I need to keep in mind after cruciate ligament surgery?
You should elevate and ice your knee immediately after the procedure. The sutures will be removed about 10 days after surgery. At that point, you may shower again.
To avoid complications, you should rest the knee for about 6 weeks after cruciate ligament reconstruction. For this time, you will receive a written sick note and forearm crutches from us. It is vital to use thrombosis prophylaxis until your leg returns to full weight-bearing. Extensive physical therapy is vital during this time to prevent muscle loss and the function of the knee.
You should schedule your return flight no earlier than 10 days after surgery. We recommend waiting about 14 days.
- Inpatient treatment: 3–4 days
- Optimal local stay: 10–14 days
- Earliest return flight: 10 days after surgery
- Recommended return flight: 14 days after surgery
- Showering permitted: 10 days after surgery
- Recommended time off work: 6–8 weeks (varies by type of job)
- Recommended removal of sutures: 10 days
- Outpatient physiotherapy: 2 weeks
- Time before being able to drive again: 6 weeks
- Low-impact exercise: 3 to 6 months after surgery
- Normal exercise: 9 months after surgery
How much is knee surgery?
In addition to the cost of knee surgery, you will also need to plan for additional costs for diagnostics, physician’s appointments and aids (e.g. forearm crutches). These will be about 1,500 to 2,000 Euro. If you plan to have outpatient physiotherapy after surgery, we will gladly obtain an estimate of costs.
You will find information about the cost of hotel lodging and any follow-up treatment at the rehabilitation clinic on the websites of the respective providers.
How can international patients schedule cruciate ligament surgery?
We will first need recent MRI images and X-rays to assess the condition of your knee. After sending these to us through our website, we will send you patient information and a binding estimate of costs within 1–2 days.
Gelenk-Klinik offers quick appointments to accommodate your preferred travel itinerary. We will gladly help you apply for a visa once we have received the down payment specified in the cost estimate. If the visa is denied, we will refund the full down payment.
We try to minimise the time between the preliminary examination and the surgery for our international patients to avoid additional travel. During your inpatient and outpatient stay our multi-lingual (English, Russian, Spanish, Portuguese) case management team will be there to assist you. We can also provide an interpreter (e.g. Arabic) at any time, at the patient’s expense. We will gladly assist you with organising transportation and lodging and provide tips for recreational activities for your family members.