Lumbar Spine (LS) Surgeries
- Causes for lumbar pain
- When is surgery a good option for lumbar pain?
- Which lumbar spine procedures does Gelenk-Klinik offer?
- Which type of physician performs lumbar spine surgery?
- Preparing surgical spine surgery
- What type of anaesthesia is used for lumbar spine surgery?
- Which aids will I need following lumbar spine surgery?
- Should I expect pain after lumbar spine surgery?
- What will my stay be like at Gelenk-Klinik?
- What do I need to keep in mind after surgery?
- Cost of lumbar spine surgery
- How can international patients schedule lumbar spine surgery?
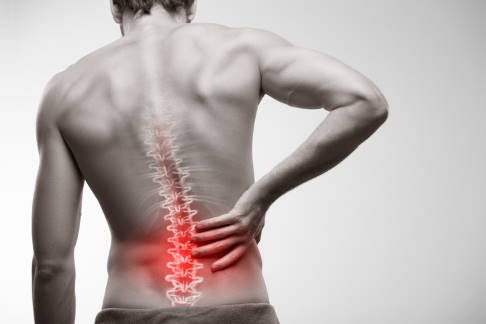 The spine is at the heart of human motion. Back pain often considerably limits quality of life. © Filip_Krstic, istock
The spine is at the heart of human motion. Back pain often considerably limits quality of life. © Filip_Krstic, istock
By far the most back pain occurs in the lowest section of the spine. The lumbar spine bears the torso’s entire weight. The vertebrae bearing this weight are rather small when compared to other areas of the spine. Walking upright puts great strain on the joints in the lumbar spine.
Every day some of the fluid in the discs which cushion and absorb is lost and they shrink. Although this fluid is restored overnight and when lying down, this process of restoration slows as we age and the discs shrink permanently.
This shrinkage causes a decline in muscle tension. The lumbar spine bulges forward and this can result in increasing hollow back which puts further strain on the back itself. The result is deep-seated back pain that can radiate in a belt-like pattern. Additionally, the movements that pass from the torso to the legs take place in the area of the lumbar spine. This involves muscular traction such as the hip flexor or the so-called adductors. This is why the back specialist must also take a close look at the pelvis and legs during the examination.
Causes for lumbar pain
Cause for low back pain:
- Herniated disc
- Spinal canal stenosis
- Lumbago
- Deformities with malposition of the spine (scoliosis, block or wedge-shaped vertebra)
- Muscular imbalance
- Inflammation (rheumatic diseases, infections)
- Osteoporosis
- Bone fractures
- Tumours and metastases in the spine
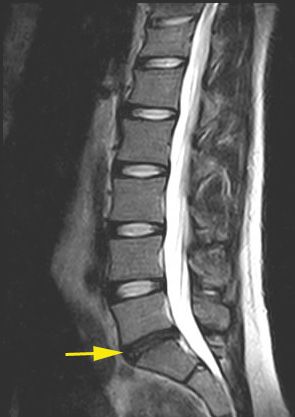 Degenerated disc with lower fluid content. © joint-surgeon
Degenerated disc with lower fluid content. © joint-surgeon
Over time, the many different stresses can also lead to permanent damage to the discs. Particularly worthy of mention here is a herniated disc in the lumbar spine. In this case, a part of the disc presses on one of the large nerve cords of the spine, which often causes typical radiating leg pain in addition to back pain.
A long unrecognised cause of back pain is so-called discogenic pain. It occurs when vessels and pain fibres grow into the disc tissue, especially into the fibrous ring of the disc. Pressure-induced back pain is the result. At an advanced stage this can result in osteochondrosis. Osteochondrosis is described as wear and tear of the disc with a reaction in the adjacent vertebrae.
Often the spine becomes increasingly unstable, resulting in movement-related pain. The spine’s response to osteophytes can then in turn cause progressive pain in the legs due to the narrowing of the vertebral canal and the nerve structures. This medical condition, referred to as spinal canal stenosis, is often the end stage of a long history of suffering from lumbar pain.
When is surgery a good option for lumbar pain?
Warning signs indicating a need for surgery:
- Bladder leakage (incontinence)
- Rectal function disorders
- Spinal paraplegia in the lower spinal marrow (so-called cauda equina syndrome)
- Paralysis
- Dysesthesia, numbness
- Considerably worsening pain resistant to treatment
Lower back pain treatment is determined by what causes the pain. Initially, general treatment approaches such as heat or cold therapy, physiotherapy, manual therapy, electricity applications as well as traditional pain therapies can alleviate or even cure the pain. In addition, the patient should ensure that their everyday activities are back-friendly. Half an hour of exercise per day prevents bad posture and can counteract back pain. If these options do not yield the desired results, special pain therapies, for example in a pain management clinic or surgery, can eliminate the cause of the back pain and further help the patient.
If pain, loss of sensation and paralysis greatly reduce the quality of life, lumbar spine surgery is a good option. Medical aspects in favour of surgery are neurological deficits (paralysis, numbness, formication) and other deficits. In many cases, early intervention is better, in order to be able to implant a prosthetic disc, for example, which reduces the pressure on the spinal cord in the lumbar spine.
Which lumbar spine procedures does Gelenk-Klinik offer?
There are different surgical procedures depending on the cause of pain in the lumbar spine.
In the case of endoscopic procedures, the surgeon works through an access point only millimetres in size without scarring the soft tissue of the spine or losing bone substance.
Minimally invasive surgeries are also referred to as “keyhole surgery”. They require minimal skin incisions and include pain management procedures and surgeries related to herniated discs. For patients, minimally invasive surgery is associated with a quicker recovery and less pain compared to a more traditional, so-called open, microsurgical procedure.
Not all spine disorders qualify for endoscopic or minimally invasive procedures. Sometimes, it becomes necessary to switch to open surgery during surgery, for example, to relieve a compressed nerve root.
The specialists at Gelenk-Klinik decide on the time and type of surgical intervention in close consultation and with consideration for the patient's personal requirements. Even the physiotherapy treatment plan following surgery is tailored to the patient.
Nucleoplasty
Nucleoplasty is an endoscopic procedure used to treat a not fully herniated disc. If the fibrous ring around the nucleus is bulging outwards and compresses the spinal cord nerves, nucleoplasty can treat this disc protrusion without open surgery. With this procedure, a high-frequency probe is inserted into the affected disc. Using an electric probe inserted under constant x-ray monitoring, the surgeon shrinks the nucleus to such an extent that it no longer presses against the spinal cord nerve. With over 80 % satisfied and pain-free patients, this procedure has an excellent success rate.
Disc prosthesis
Artificial discs have been a reliable and common treatment for degenerated discs for over ten years now. The disc prosthesis offers a particularly promising alternative to the previously commonly used fusion (spondylodesis) of individual vertebrae. It is intended to restore the natural mobility and function of the disc. The disc prosthesis is intended to minimise or even eliminate symptoms associated with disc degeneration and a herniated disc, chronic back pain, and neurological losses. Replacing the natural disc, the prosthesis protects the spine from further degeneration, stabilising it in the long term.
Fusion (spondylodesis)
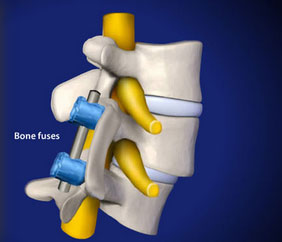 The fusion surgery of vertebrate bodies to stabilize displaced vertebrae has a long history. © Viewmedica
The fusion surgery of vertebrate bodies to stabilize displaced vertebrae has a long history. © Viewmedica
Progressive wear of the spine often reduces the space between vertebrae. The space between the vertebrae narrows. The spine becomes unstable and the vertebrae shift forward, backward, or to the side. If all conservative treatment options have been exhausted and even minimally-invasive procedures are no longer promising, fusing the painful area of the spine is the last resort. A combination of screws and small connecting rods immobilises the affected area of the spine. With today’s techniques, this can typically be done as a minimally-invasive procedure through small skin incisions. However, this spondylodesis typically does not completely eliminate symptoms, but rather improves pain in the lumbar spine.
Which type of physician performs lumbar spine surgery?
Here at Gelenk-Klinik we believe a close relationship between the physician and their patient is important. Meaning, you will be in the care of your treating physician from the initial appointment until after the spine surgery. This physician is also responsible for your after-care. So, you will have one contact person who will be assigned to you throughout your stay at Gelenk-Klinik. Our specialist for back pain and spine surgery is the experienced neurosurgeon Dr David-Christopher Kubosch.
Preparing surgical spine surgery
First the physician will perform a thorough medical examination. Diagnostic imaging is used to help understand the results. Medical examination means: Discussing the medical history and a physical examination. Diagnostic imaging means: Taking x-rays lying down and standing, so weight-bearing. Furthermore, an MRI (magnetic resonance imaging) is important to determine the condition of the discs and nerves in the spinal column. A bone density measurement may also be performed to determine the stability of the bones and to rule out osteoporotic changes.
After determining the patient’s suitability for surgery, the treating physician will discuss the procedure and possible complications of lumbar spine surgery with the patient. In addition, there will be a detailed discussion with the anaesthetist, who will again review the patient’s health condition with respect to anaesthesia. Once approved by the anaesthetist and the surgeon, the surgery can typically be performed the day after the examination.
What type of anaesthesia is used for lumbar spine surgery?
Spine surgery is typically performed under general anaesthesia. The anaesthetist will inject a combination of anaesthetics individually tailored to your body. You will feel no pain during the surgery and will not be aware of the procedure. An experienced anaesthetist will be present throughout the procedure, monitoring your vital functions and ensuring you do not wake up during the surgery.
Which aids will I need following lumbar spine surgery?
In the first days following surgery it will be important to rest your lumbar spine and move it as little as possible. We will supply you with a back brace to wear for 2 to 6 weeks to ensure this. This will stabilise your lumbar spine and prevent any abrupt movements.
Should I expect pain after lumbar spine surgery?
Every surgical procedure may cause pain. We always try to minimise pain as much as possible. Once the general anaesthesia wears off, you will receive pain medication by IV or in form of tablets. Our goal is for you to experience as little pain as possible.
What will my stay be like at Gelenk-Klinik?
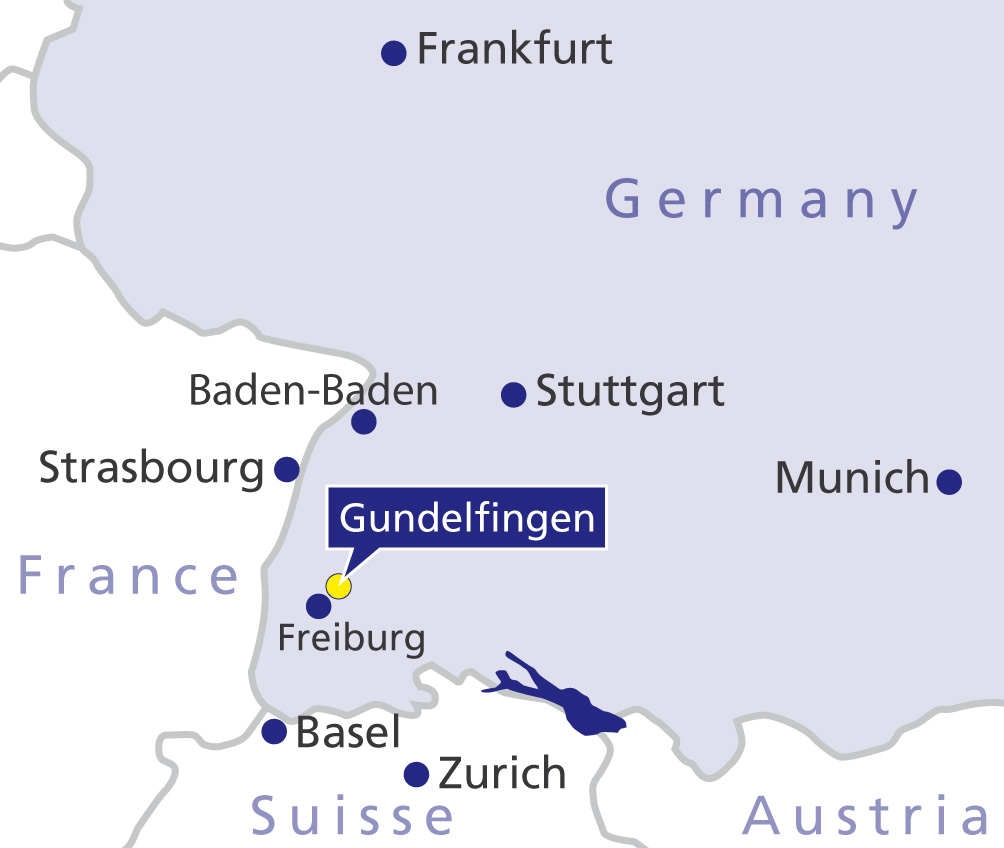
 Private room in the Gelenk-Klinik in Gundelfingen, Germany. © joint-surgeon
Private room in the Gelenk-Klinik in Gundelfingen, Germany. © joint-surgeon
During your inpatient stay at Gelenk-Klinik you will have a single-occupancy room. The room has a bathroom with a shower and WC. All rooms include towels, a bathrobe and slippers. They further include a mini-bar and a safe. All rooms also have a television. You only need to bring your personal medication, comfortable clothes and sleepwear. After surgery, you will receive 24-hour care from experienced nursing staff, international patient care team and experienced physiotherapists. The inpatient stay following the procedure typically lasts 3 days. Your family members can stay at a hotel within walking distance (300 m). We will help you to make the reservations.
What do I need to keep in mind after surgery?
After surgery you should rest your spine and avoid any sudden movement. Depending on the physician’s instructions you will receive manual therapy to resolve functional disorders of the musculoskeletal system from our experienced physiotherapists. After about 6 weeks of rest, you will typically be able to return to work and exercise. The sutures do not need to be removed, as we use special absorbable sutures. So, you will already be able to shower 7 days after surgery.
- Inpatient treatment: 2–5 days
- Optimal local stay: 10–14 days
- Earliest return flight: 7 days after surgery
- Recommended return flight: 14 days after surgery
- Showering permitted: 7 days after surgery
- Recommended time off work: 4 weeks (varies by job)
- Recommended removal of sutures: None (absorbable sutures)
- Time before being able to drive again: 2 weeks
- Outpatient physiotherapy: 2 weeks
Cost of lumbar spine surgery
In addition to the cost of surgery you will also need to plan for additional costs for diagnosis, physician’s appointments and aids. If you plan to have outpatient physiotherapy in Germany after surgery, we will gladly schedule the appointments with the physiotherapists and obtain an estimate of costs.
You will find information about the cost of hotel lodging and any follow-up treatment at the rehabilitation clinic on the websites of the respective providers. We will gladly assist you with planning your rehabilitation stay.
How can international patients schedule lumbar spine surgery?
We will first need recent MRI images, particularly x-rays of the lumbar spine to assess the condition of the discs, vertebrae and facet joints. After sending these to us through our website, we will send you patient information including proposed treatment and a binding estimate of costs within 1–2 days.
Gelenk-Klinik offers quick appointments for international patients to correspond with your preferred travel itinerary. We will gladly help you apply for a visa once we have received the down payment specified in the cost estimate. If the visa is denied, we will promptly refund the full down payment.
We try to minimise the time between the preliminary examination and the surgery for our international patients to shorten your stay and avoid additional travel. During your inpatient and outpatient stay our multi-lingual (English, Russian, Spanish, Portuguese) case management team will be there to assist you. We can also provide an interpreter (e.g. Arabic) at any time, at the patient’s expense. We will gladly assist you with organising transportation and lodging and provide tips for recreational activities for your family members.