Cartilage cell transplant for osteoarthritis of the knee
- Goals of a cartilage cell transplant for osteoarthritis of the knee
- Who is a knee cartilage transplant suitable for?
- Procedure for harvesting cartilage
- Which doctors perform cartilage cell transplants?
- What is the expected success rate of a cartilage cell transplant?
- What happens prior to surgery?
- What happens during the cartilage transplant surgery?
- What type of anaesthetic is used for a cartilage cell transplant?
- Should I expect pain after the surgery?
- What will my stay be like at Gelenk-Klinik?
- What do I need to keep in mind after surgery?
- What is the cost of a cartilage cell transplant?
- Is a cartilage cell transplant right for me?
- How can international patients schedule a cartilage cell transplant?
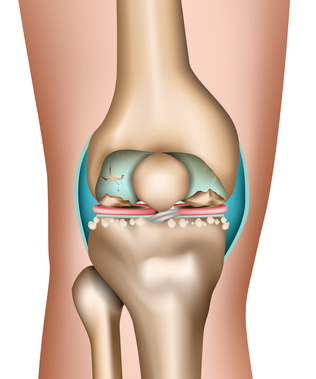 There are many causes for painful worn cartilage in the knee joint: arthritis, arthrosis, traumas with bone- or cartilage lesions or metabolic disorders like gout or hemochromatosis. © bilderzwerg,fotolia
There are many causes for painful worn cartilage in the knee joint: arthritis, arthrosis, traumas with bone- or cartilage lesions or metabolic disorders like gout or hemochromatosis. © bilderzwerg,fotolia
Osteoarthritis (worn cartilage) is the most common joint condition. The most common form of osteoarthritis is osteoarthritis of the knee. Osteoarthritis of the knee causes chronic pain and limits movement. The cartilage in the knee wears away over many years. Since the cartilage has no nerve endings (pain sensors), the damage is only noticed when the defects already affect the bone beneath the cartilage.
A cartilage transplant, or cartilage cell or chondrocyte transplant, is a new surgical procedure: in which cartilage damage is repaired using cartilage cells from the patient’s own body. Few knee specialists in Germany successfully perform this procedure. The founder of the Gelenk-Klinik was the first physician in the world to perform an entirely arthroscopic cartilage transplant of the knee. He co-developed this procedure and trained other physicians in this surgical procedure.
The goals of a cartilage cell transplant of the knee:
- Reduce pain due to knee osteoarthritis
- Restoring the ability to bear weight and play sports
- Improve flexibility
- Restore the cartilage layer
- Prevent a joint replacement
- Preserve the joint and prevent osteoarthritis of the knee
Who is a knee cartilage transplant suitable for?
A cartilage transplant is not always a suitable treatment for osteoarthritis of the knee. If the cartilage defect in the knee is too severe, it is usually too late. In this case we would instead propose a joint-preserving partial knee replacement or a full knee replacement. There are several prerequisites for a successful cartilage transplant:
- A straight joint axis without deformity (severe knock-knees or bow legs)
- No loose bodies (tissue which separated due to the cartilage defect in the knee)
- Preserved menisci, at least for the most part
- Cartilage only defective on one of the two joint surfaces
Typical indications for transplanting cartilage cells (chondrocytes) are local cartilage defects inside the knee.
What are the ideal conditions for transplanting cartilage cells into the knee?
- Patient aged 15–55 years
- Defect size up to 10 square centimetres with healthy cartilage remaining around the defect.
- The knee should be stable, i.e. the ligaments intact.
- Preferably no abnormal strain on the joint, e.g. due to obesity.
Although this method is typically only recommended for patients up to age 55, the biological age, not the calendar age of the patient is crucial. In some cases, cartilage transplants are even performed on patients over 65 years if the criteria are met. We require recent MRI scans and X-rays to assess whether your specific case qualifies for this procedure. The knee specialist can often only determine during the procedure whether a partial prosthesis or a cartilage transplant is the best treatment option.
If a cartilage cell transplant is not an option for you, there are other options (e.g. a partial prosthesis using Hemicap system, a Repicci prosthesis or a complete replacement) to treat osteoarthritis of the knee.
Procedure for harvesting cartilage for a cartilage transplant
 After harvesting cartilage from a healthy section of the knee the cells are grown in a specialised cell culture lab. © Istockphoto.com
After harvesting cartilage from a healthy section of the knee the cells are grown in a specialised cell culture lab. © Istockphoto.com
Step 1: Harvesting a cartilage sample (biopsy specimen) from the knee
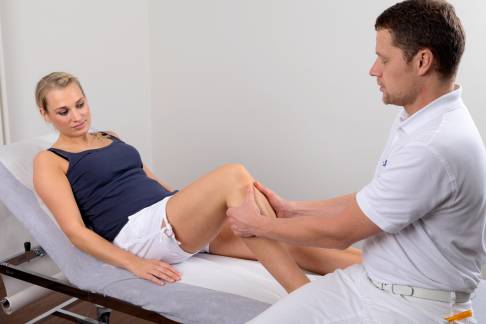
The surgeon will first harvest cartilage from the patient’s body using arthroscopy at our Gelenk-Klinik. The cartilage tissue, about the size of a grain of rice, is removed from a healthy section of the knee which does not bear much weight. The cartilage cells are isolated from this harvested tissue in a highly specialised cell culture lab and cultivated, i.e. grown, under sterile conditions.
This procedure takes about 30 minutes. The next day, approximately 120–150 ml of blood is drawn from a vein in the patient’s arm. The laboratory uses this blood to obtain the serum (liquid part of the blood).
Step 2: Growing cells in the laboratory
The harvested rice-grain-sized cartilage specimen along with the patient’s blood sample is taken to the laboratory. The cartilage cells are isolated from the tissue sample and grown in the patient’s blood serum under sterile conditions. This procedure completely rules out any contact with proteins or blood components foreign to the body.
At the end of the production process, which typically takes 6-8 weeks, small spherical cell aggregates have formed which contain hundreds of thousands of augmentable cartilage cells. The cartilage cells are transported back to the clinic within hours inside special refrigerated containers to preserve the quality of the cells.
Which doctors perform knee cartilage cell transplants?
Here at Gelenk-Klinik we believe a close relationship between physicians and patients is important. This means you will be in the care of your attending knee specialist from your initial appointment until after the cartilage cells have been transplanted. This doctor is also responsible for your aftercare. You will therefore have one contact person who will be assigned to you throughout your stay at Gelenk-Klinik. Our knee cartilage transplant experts are Professor Sven Ostermeier and PD Dr Bastian Marquaß.
What is the expected success rate of a cartilage cell transplant?
Cartilage cell transplants have been performed for about 25 years. Studies have shown the method significantly improves the cartilage surface in the joint. After the cartilage transplant the replacement cartilage cannot be distinguished from the original cartilage. The procedure can alleviate pain and restore mobility.
The founder of the Gelenk-Klinik is one of the world’s leading specialists in the field of cartilage cell transplant, working at the Gelenk-Klinik. He was the first physician on an international level who performed a completely arthroscopic cartilage transplant, which means with minimal intervention and virtually without scars. Professor Ostermeier and PD. Dr Marquaß are leaders in researching cartilage treatments and have published numerous papers on this topic.
What happens prior to surgery?
The physician will first perform detailed medical diagnostics to obtain a good overall picture. In addition to reviewing your medical history and a medical examination, this also includes X-rays whilst bearing weight and MRI scans (Magnetic resonance imaging) to assess the extent of the cartilage damage.
After determining the patient is fit for surgery, the attending physician will explain the procedure and possible complications of surgery. The patient will also meet with the anaesthetist, who will again review in detail whether the patient is healthy enough for anaesthesia. Once approved by the anaesthetist and the surgeon, the operation can typically be performed the next day.
What happens during the cartilage transplant surgery?
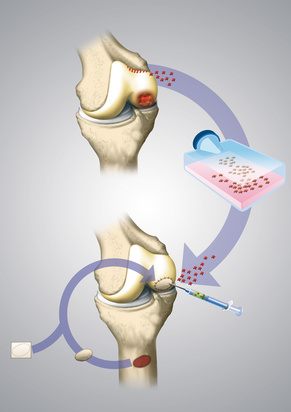 The cartilage cells are harvested arthroscopically. After they were grown at a specialised cell lab the doctor implants them in a minimally invasive operation. © dissoid, Fotolia
The cartilage cells are harvested arthroscopically. After they were grown at a specialised cell lab the doctor implants them in a minimally invasive operation. © dissoid, Fotolia
The cartilage cells which were grown at the laboratory are mostly implanted arthroscopically, i.e. as minimally invasive as possible. Only minimal skin incisions are needed to insert the necessary instruments in the knee.
The surgeon will first remove damaged cartilage tissue from the knee and then implant the cultured cartilage spheres (chondrospheres) into the prepared defective area. There they will immediately adhere to the bone and form connective tissue typical for cartilage to fill in the defect after a few weeks.
Once the cartilage cells establish contact with the prepared cartilage defect, their connective molecules (adhesion proteins) form a mechanically stable adhesion to the bone after roughly 10 minutes. The cartilage cells grow into the defect until it is completely filled in. The procedure is performed at the Gelenk-Klinik and takes about 30–60 minutes unless other corrections, e.g. to the cruciate ligaments or the meniscus are required.
To ensure a successful outcome of the cartilage transplant, it is furthermore important that problems which caused the cartilage damage (e.g. misalignments, cruciate ligament ruptures, meniscus damage, etc.), are identified and treated, which typically occurs at the same time as the cartilage transplant. In this way, the patient only needs to undergo one round of slightly time-consuming after-care and resting.
What type of anaesthetic is used for a cartilage cell transplant?
The cartilage cell transplant is typically performed under general anaesthesia. However, we can also perform it under spinal anaesthesia to reduce the risks of general anaesthesia. In this case the anaesthetist injects the anaesthetic into the vertebral canal of the lumbar spine. Here, the patient is conscious during surgery. Our anaesthetists are very experienced in both methods and choose the option best suited for you and your requirements during a pre-operation discussion.
Should I expect pain after the surgery?
Any procedure causes pain, but we always strive to minimise it. The anaesthetist will often use a so-called nerve block before the surgery, numbing the respective knee for approximately 30 hours. This step alone manages the majority of the pain, and any residual discomfort can then be easily treated with typical medication. Our goal is for you to experience as little pain as possible.
What will my stay be like at Gelenk-Klinik?
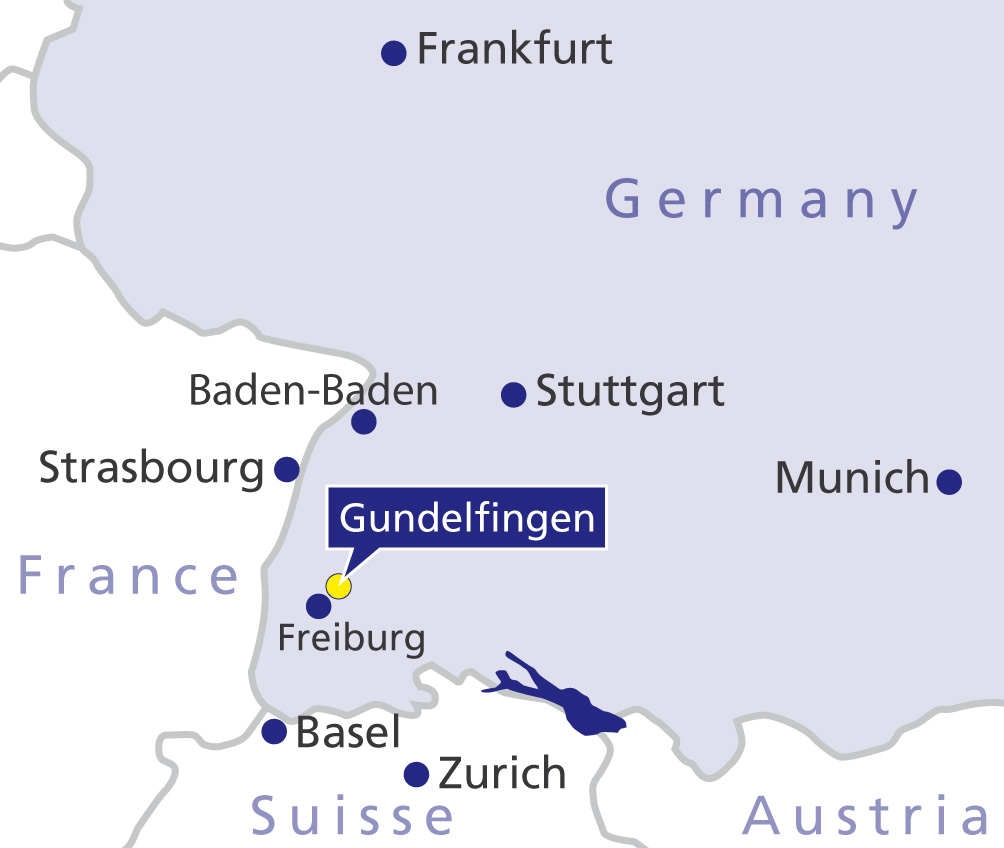
 Private room in the Gelenk-Klinik in Gundelfingen, Germany
Private room in the Gelenk-Klinik in Gundelfingen, Germany
During your inpatient stay at Gelenk-Klinik you will have a single-occupancy room. The room has a bathroom with shower and toilet. All rooms include towels, a bathrobe and slippers. They also feature a mini-bar and a safe. All of the rooms are moreover fitted with a television.
You only need to bring your personal medication, comfortable clothes and sleepwear. After surgery you will receive 24-hour care from experienced nursing staff and experienced physiotherapists. The inpatient stay is typically 3 days after the procedure. There is a hotel within walking distance where your family members can stay. We are happy to make reservations for you.
What do I need to keep in mind after surgery?
You should elevate and ice your knee immediately following the procedure. The stitches will be removed about 7 to 12 days after the surgery. Once these are removed, you can also shower again.
You should rest your knee and avoid weight-bearing for approx. 6 weeks to prevent complications. You will receive a special M4-orthosis to prevent the knee from bending too much (depending on where the cartilage defect was situated). We will also provide you with a medical sick leave and crutches for this period. Thrombosis prophylaxis are imperative during the time you are unable to put your full weight on the leg. Extensive physiotherapy is very important during this stage to prevent muscle loss and maintain the function of the knee.
Physiotherapy, especially with manual therapy and lymphatic drainage, helps to reduce swelling after the procedure.
You should plan your return flight at least 10 days after surgery. We recommend about 14 days.
 To maintain the function of the knee and to prevent swelling physiotherapy is very important. © Elnur, Fotolia
To maintain the function of the knee and to prevent swelling physiotherapy is very important. © Elnur, Fotolia
Recommendations for after arthroscopy (1st procedure)
- Inpatient treatment: 2 days
- Optimal length of stay on the premises: 7 days
- Earliest return flight: 7 days after surgery
- Recommended return flight: 10 days after surgery
- Showering permitted: 5 days after surgery
- Recommended time off work: 2 weeks
- Recommended removal of stitches: 5 days
- Time before able to drive again: 2 weeks
Recommendations following cell implant, which, if required, corrects the cause of the cartilage damage (2nd procedure)
- Inpatient treatment: 3 days
- Complete rest of the operated leg: 6 weeks
- Then partial weight-bearing of the operated leg: 6–8 weeks
- Optimal length of stay on the premises: 10 days
- Earliest return flight: 10 days after surgery
- Recommended return flight: 14 days after surgery
- Showering permitted: 7 days after surgery
- Recommended time off work: 6 weeks
- Recommended removal of stitches: 7–12 days
- Time before able to drive again: 6–12 weeks
What is the cost of a cartilage cell transplant?
In addition to the cost of surgery you also need to plan for further costs for diagnosis, doctor’s appointments and temporary supports (e.g. crutches). These amount to between € 1500 and € 2000. If you plan to have outpatient physiotherapy in Germany after surgery, we will gladly obtain an estimate of costs.
You will find information about the cost of hotel lodging and any follow-up treatment at the rehabilitation clinic on the websites of the respective providers.
Is a cartilage cell transplant right for me?
We require recent MRI scans and X-rays to be able to fully assess the cartilage damage in your knee. We will use these scans to determine if you qualify for the procedure. We will gladly also advise you on alternative treatment options if your specific case does not qualify for a cartilage transplant.
How can international patients schedule a cartilage cell transplant?
We firstly require recent MRI imaging and X-rays to be able to fully assess the condition of your knee. After sending these to us via our website, we will send you patient information including proposed treatment and a binding estimate of costs within 1–2 days.
Gelenk-Klinik offers appointments to correspond with your preferred travel itinerary. We will gladly help you apply for a visa once we have received the down-payment specified in the cost estimate. If the visa is denied, we will refund the full down-payment.
We try to minimise the time between the preliminary examination and the surgery for our international patients to avoid additional travel. During your inpatient and outpatient stay our multi-lingual (English, Russian, Spanish, Portuguese) case management team will be there to assist you. We can also provide an interpreter (e.g. Arabic) at any time, at the patient’s expense. We will gladly assist you with organising transportation and lodging and provide recreational tips for your family members.